Follow Up on Unpaid Encounters with Insurance Balances
How can you track your practice’s insurance A/R, know where your money is, and make sure payers respond to your claims? Use the Unpaid Encounters worklist in the Insurance Balances tool to follow up on unpaid claims.
Video: Watch Follow Up on Unpaid Encounters with Insurance Balances to learn more.
Contents
- 1 Open and Review the Unpaid Encounters Worklist
- 2 Troubleshoot a Specific Encounter
- 3 Check the Payor’s Status on a Claim
- 4 Organize Your Insurance A/R By Status
- 5 Assigned an Unpaid Encounter for Followup
- 6 Add a New Encounter Billing Note
- 7 View More Encounter Details and the Encounter’s Claim History
- 8 Edit Encounter Details and Submit a New Claim
Open and Review the Unpaid Encounters Worklist
To review encounters with unpaid insurance balances, open the Insurance Balances tool and visit the Unpaid Encounters tab.
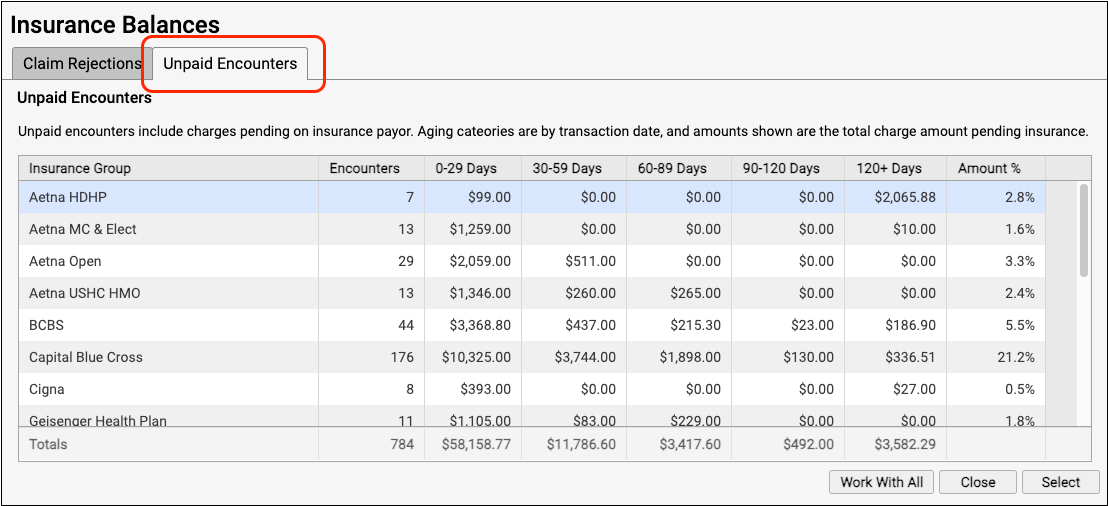
The Unpaid Encounters overview shows you total insurance balances, for each payor, aged from the date of service.
Double-click on a single insurance group or click "Work With All" to see unpaid encounters with charges pending insurance.
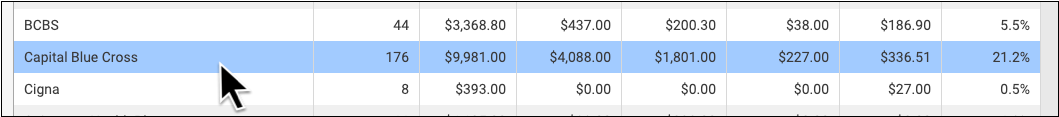
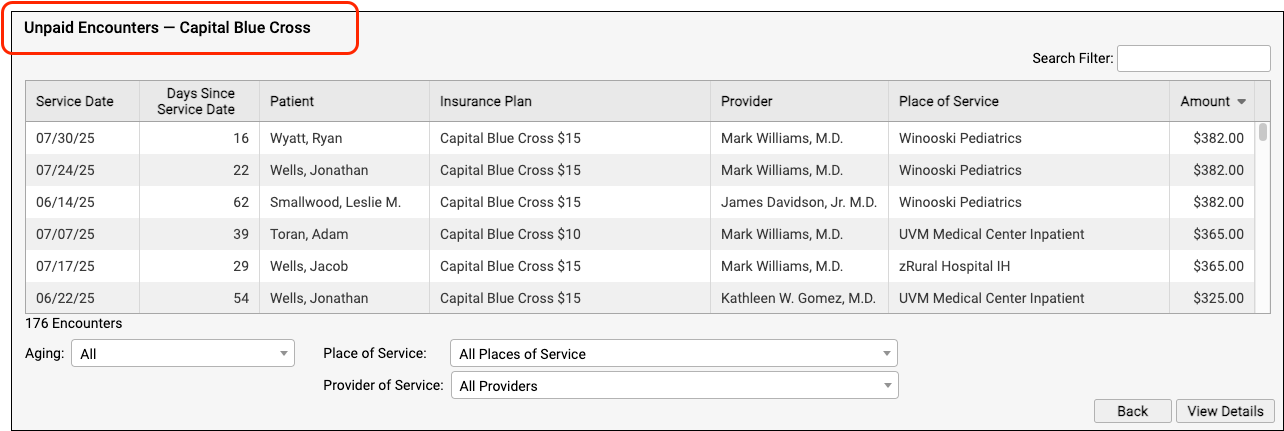
Jump to an Aging Category: You can optionally double-click on a specific aging category for a specific insurance group.
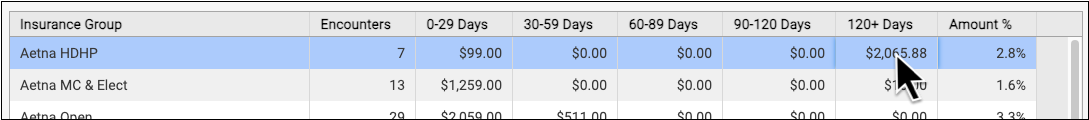
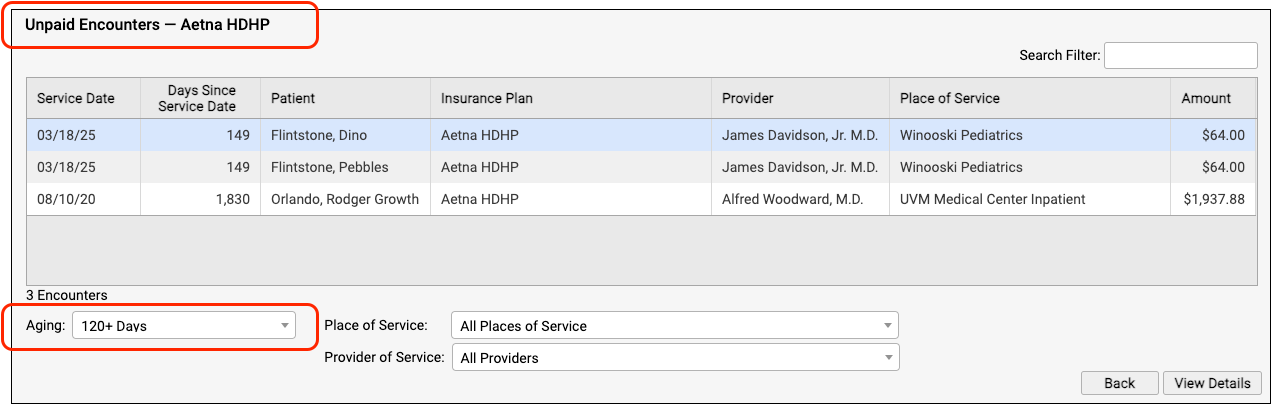
On the Unpaid Encounters worklist, you can see the date of service, the number of days since the date of service, the patient, the specific insurance plan, the provider of service, the place of service, and the amount due.
You can filter the list to isolate the specific unpaid claims that you need to work on. You can specify an aging category, a place of service, a provider of service, the billing encounter status, and the assigned user.
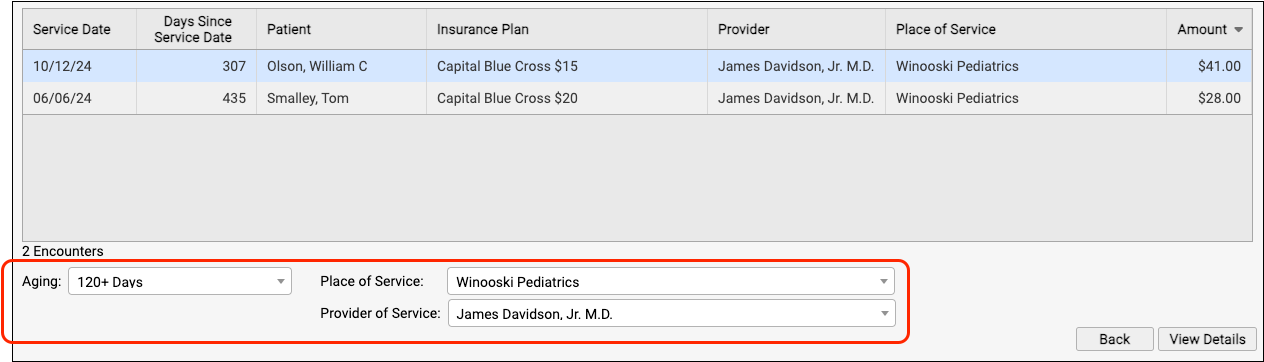
You can click on the header of any column to sort the encounters and use the Search field to filter the list down to a search term. By using these tools you can find specific groups of encounters or work down the list in a particular order.
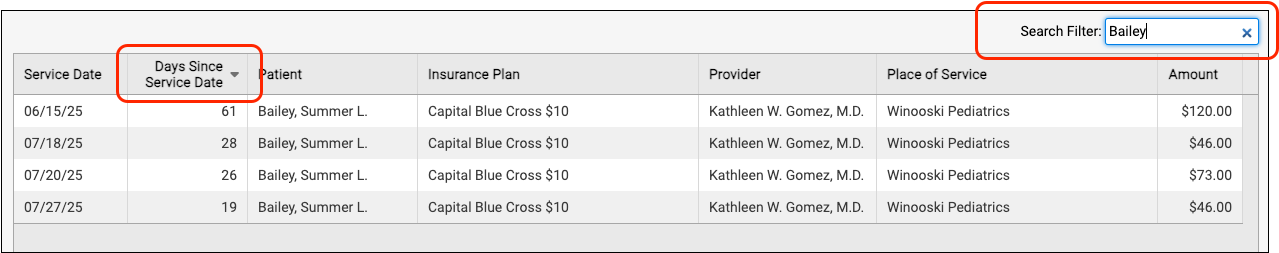
By monitoring your practice's insurance A/R on the Unpaid Encounters worklist, you can stay on top of your receivables and ensure that no claims slip through the cracks.
Troubleshoot a Specific Encounter
Double-click on an encounter to see more details.

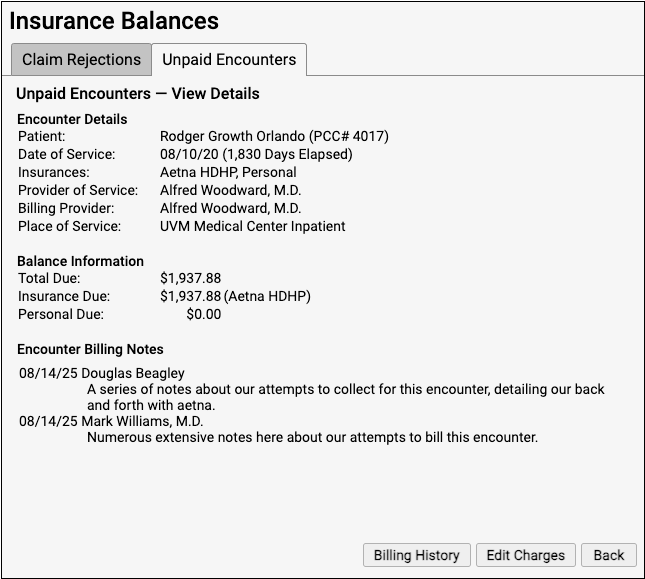
The Unpaid Encounters – View Details screen provides information that will help you review and resolve billing issues with an encounter.
-
Encounter Details: The Encounter Details section summarizes basic billing information about the encounter, including both the Provider of Service and if an overriding “Billing Provider” was used on the claim.
-
Balance Information: The Balance Information section displays how much is outstanding for the encounter, how much is pending the payor, and how much is the family’s responsibility.
-
Encounter Billing Notes: If you or someone at your practice has entered encounter billing notes (sometimes called “visit billing notes” or “oops notes”), the Encounter Billing Notes section will display those notes. If you’ve contacted the payor and submitted a claim multiple times, you can review your practice’s notes to better understand the history of the rejection.
As you work with a specific encounter, you can query the payor for claim status, organize encounters by assigning a status or staff member, update encounter billing notes, review account history, edit charges and other details of the encounter, and queue up a new claim. Read below to learn more.
Check the Payor’s Status on a Claim
Has your claim been received by the payor? Have they adjudicated it yet? What’s the status? You can click a button and instantly receive a claim status report from the payor. Instead of opening the payor’s website or calling them, you can read the payor’s latest claim status right in PCC EHR.
PCC EHR Only, Participating Payors Only: Real-time claim status is available from participating payors for claims submitted through the PCC EHR Claims tool. If you use PCC’s legacy Practice Management suite, Partner, check out Submit Claims and get in touch if you’d like help making the transition or have questions about a specific payor.
To ask the payor for status on a claim, open the encounter in the Unpaid Encounters. Then click “Request Claim Status” to query the payor.
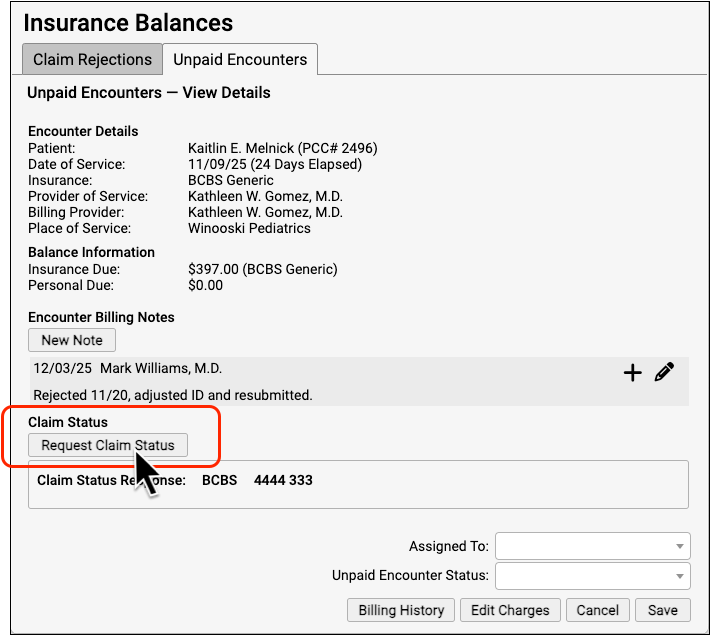
If the payor is in compliance with claim status standards, they will return a result for that encounter, and PCC will format and display the result.
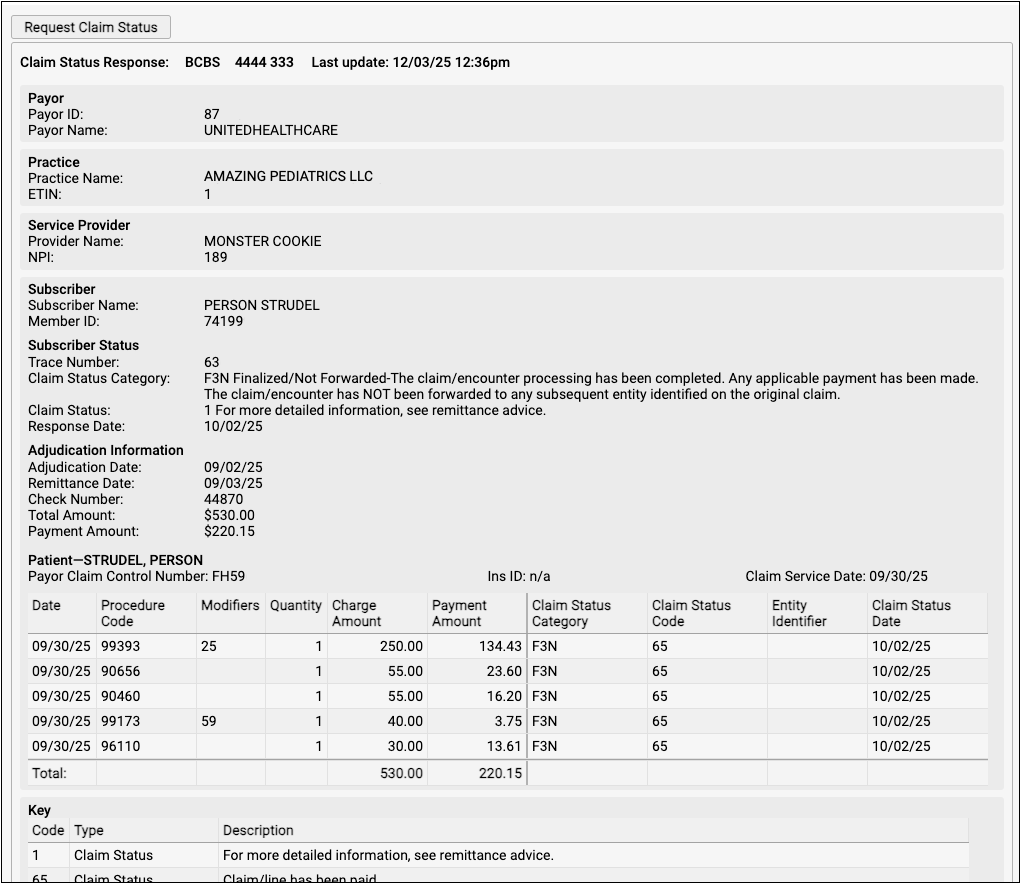
To see a claim status request in action, in the context of the Unpaid Encounters worklist, watch Follow Up on Unpaid Encounters with Insurance Balances.
Payor Usage Limits: Most payors do not provide claim status information until seven days after a claim has been submitted. Some payors will not respond to a second query within twenty-four hours. PCC can’t control whether a payor will respond, but you can follow these guidelines to prevent disappointment when you are seeking information on an unpaid claim.
Organize Your Insurance A/R By Status
As you work on the Unpaid Encounters worklist in the Insurance Balances tool, you can mark encounters with a status, such as “Waiting on Payor” or “Under Review”. Then you can track, organize, and filter your A/R by that status.
While viewing an encounter’s details, use the Encounter Status menu to set the status for an unpaid encounter.
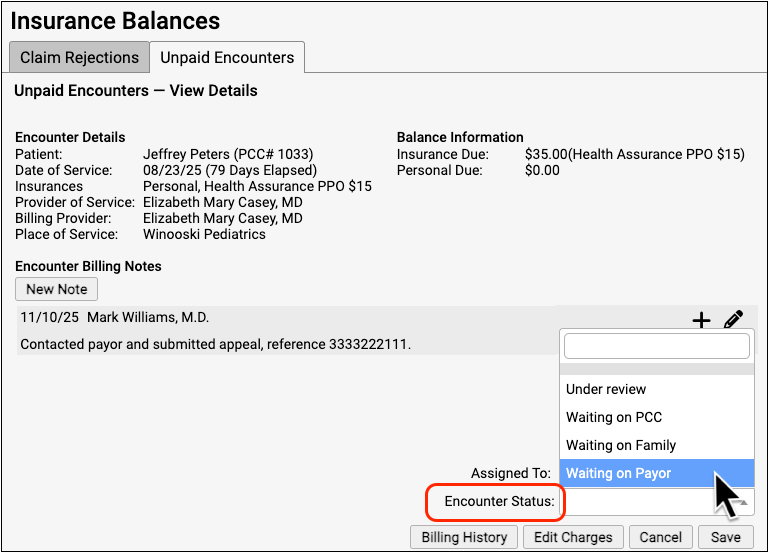
Back on the worklist, you can use filters, column sorting, and search to organize the Unpaid Encounters worklist by status.
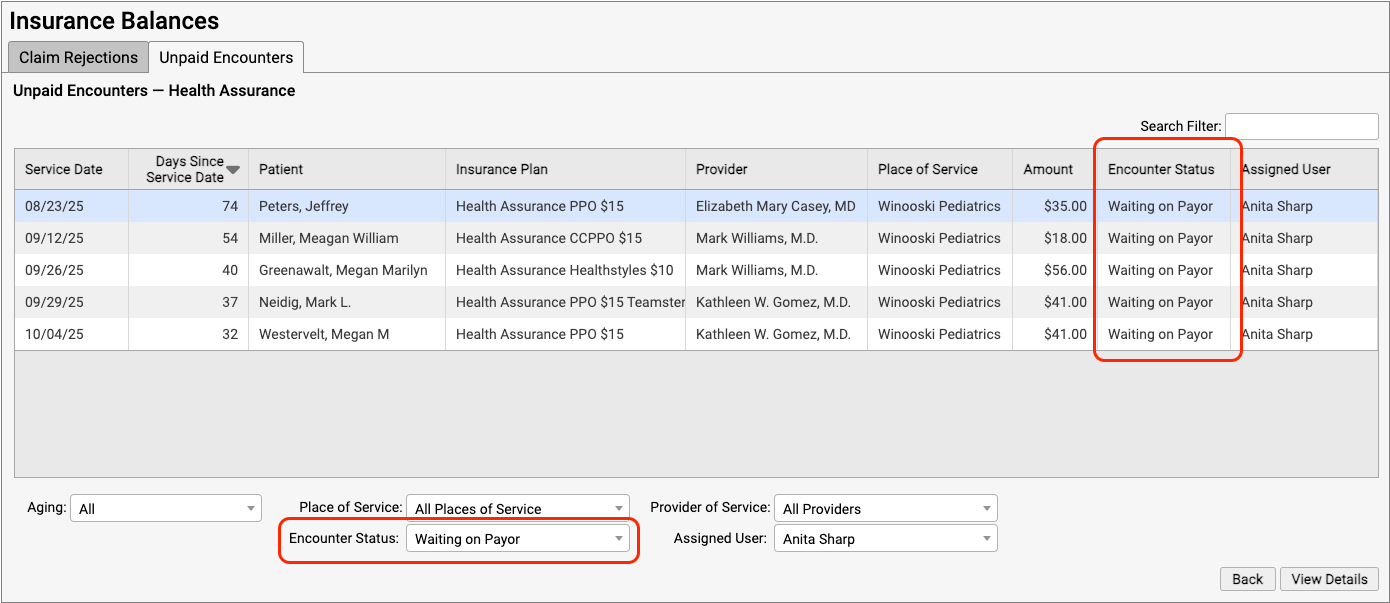
Statuses make it easier to track, organize, and filter your insurance A/R so you can address the needs of every unpaid claim.
Assigned an Unpaid Encounter for Followup
Do you need to make sure your practice follows up on an encounter? You can assign it to yourself or another biller at your practice.
Click on the Assigned To menu to assign an unpaid encounter to someone at your practice.
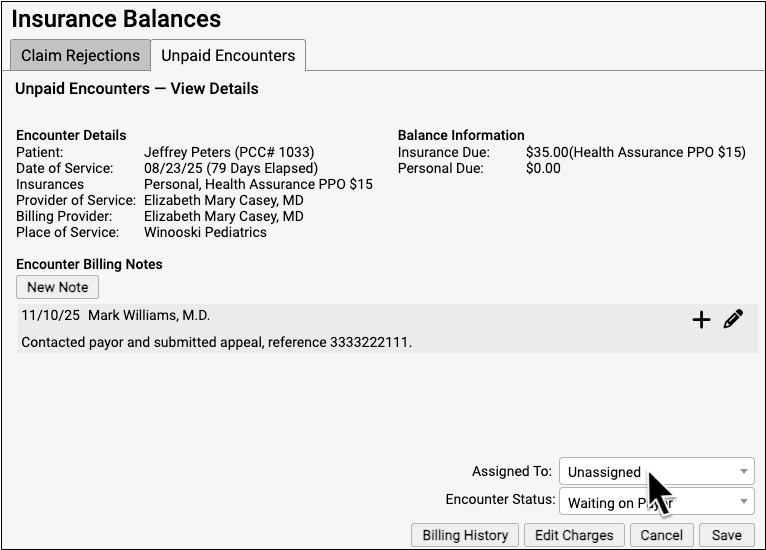
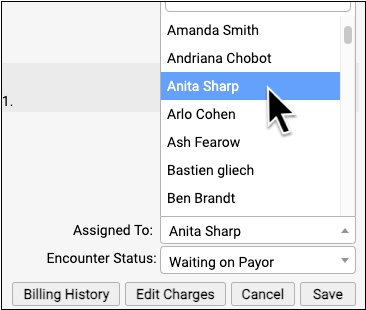
You can then use filters, column sorting, and search to organize the Unpaid Encounters worklist by assigned user.
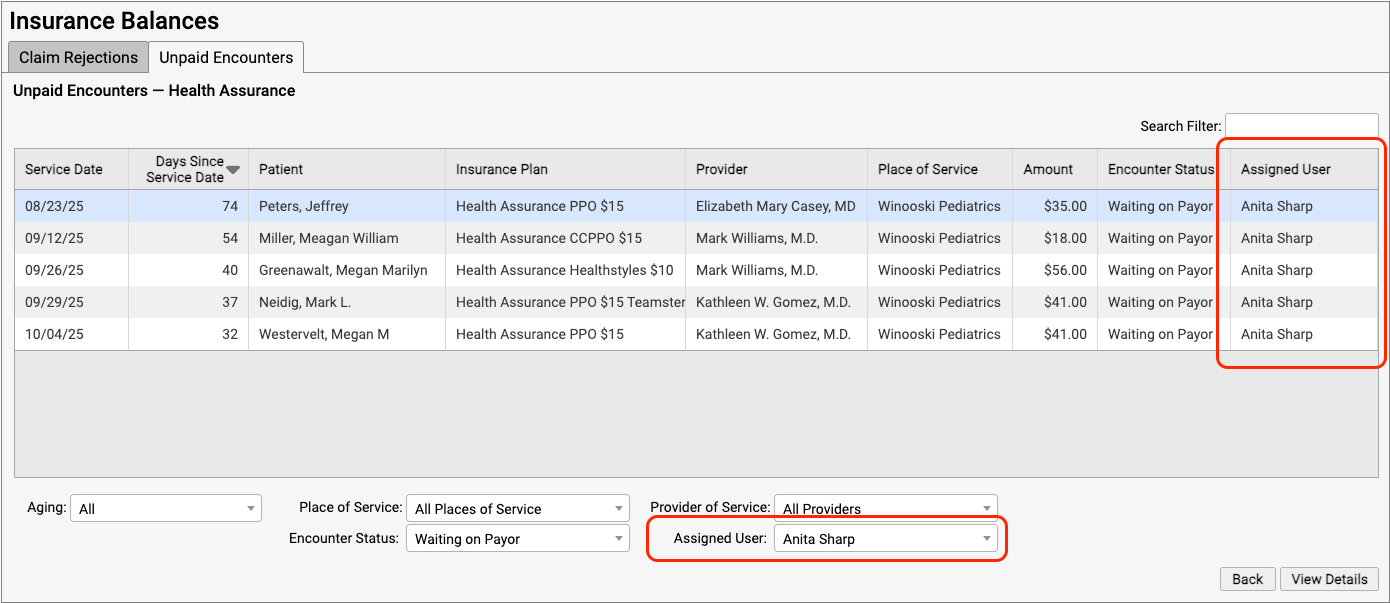
Assigning a user helps ensure your practice will followup on every unpaid claim.
Add a New Encounter Billing Note
As you work on an encounter, its billing notes appear on the detailed view.
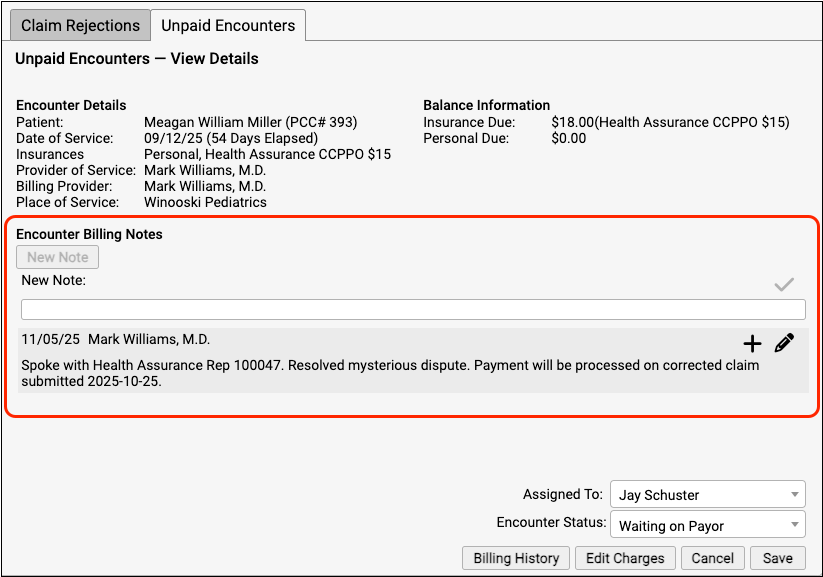
You can add a new note or followup note or edit an existing note.
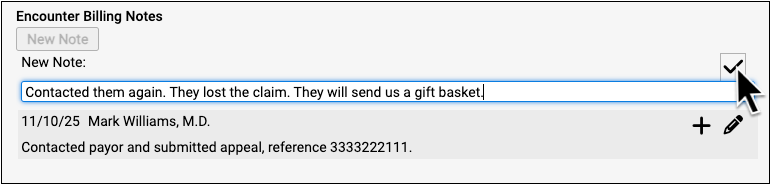
When you respond to a rejection or follow up on an appeal, the encounter billing notes help you understand what’s been done so far and record your actions as your practice seeks payment for the encounter.
View More Encounter Details and the Encounter’s Claim History
Did a claim go out? Has the payor responded? You may want to dig deeper and review charges, payments, and claim history for the encounter. Click “Billing History” to review more encounter details.
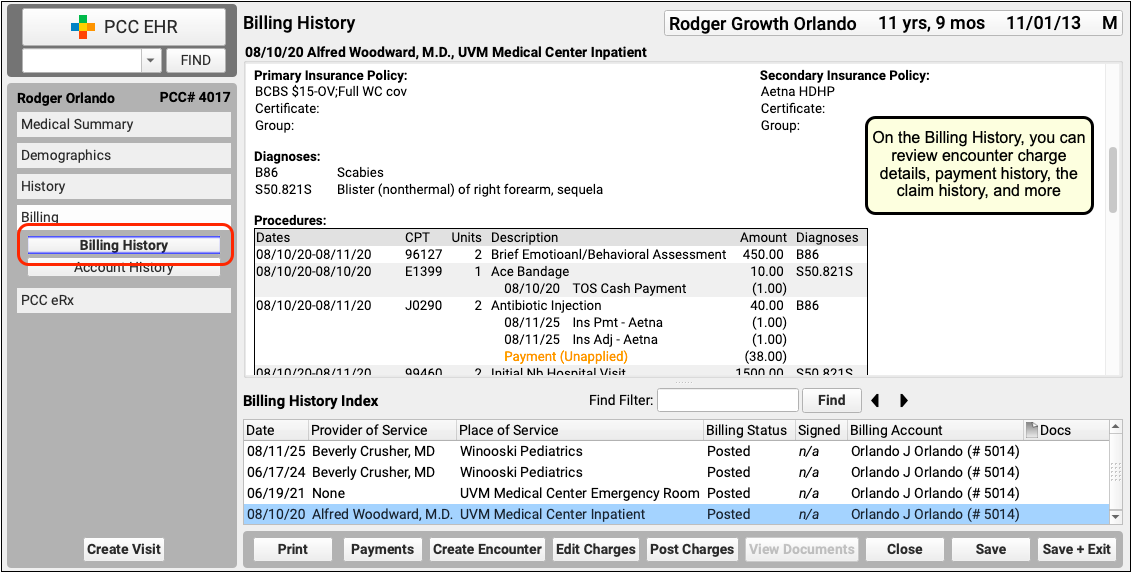
On the Billing History for the encounter, you can review full charge and payment details. The Claim History shows you all insurance billing activity and includes links to review the payor acknowledgements, posted ERAs, and more.
Review Patient Policies, the Complete Account History, and More
If you need to review more information about the patient and the account, you can navigate to other sections of the chart. For example, after clicking "Billing History", click "Demographics" to review insurance policies.
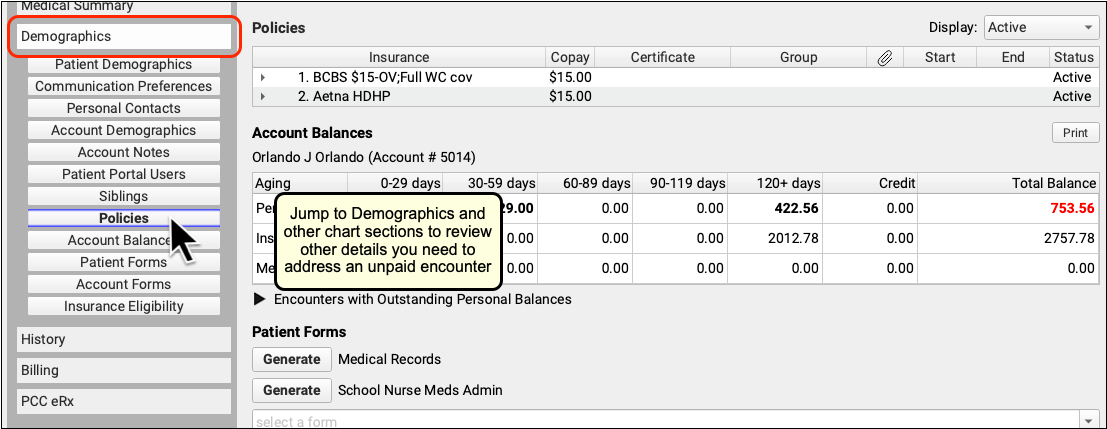
Or, to see the encounter and all financial transactions for the patient's billing account, visit the Account History.
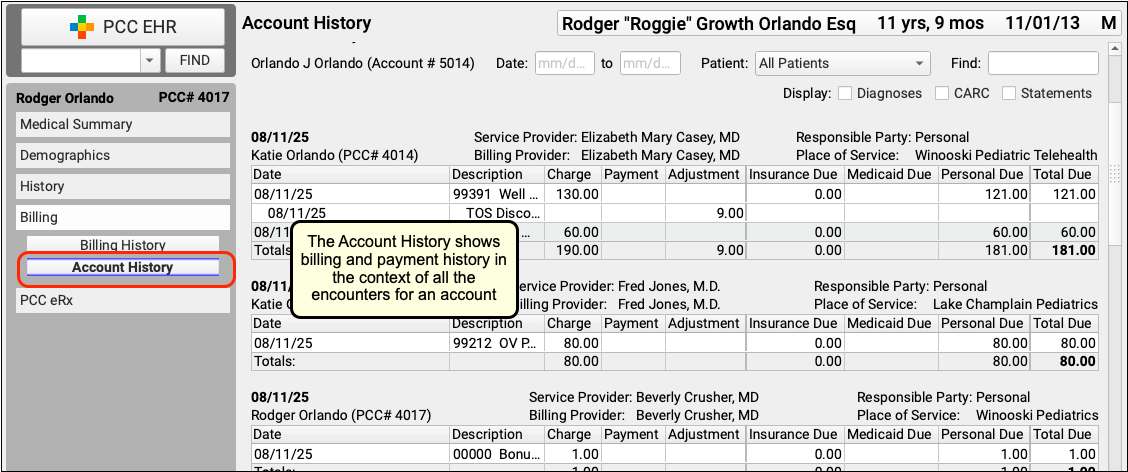
By reviewing the full account history, you can see every event linked to each encounter and also understand the encounter in the context of the family's billing record.
Review Eligibility for the Encounter's Date of Service
If you want to check if there are eligibility records for an encounter's date of service, click "Edit Charges" and then "Patient Details" to see the eligibility component for that encounter.

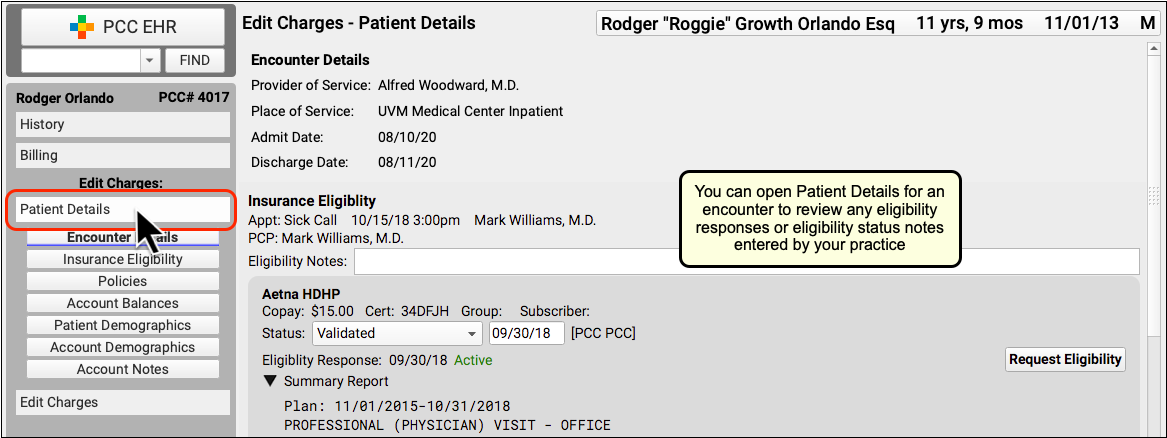
If your practice confirmed eligibility for the patient, either automatically or manually, you can review the results and any notes added at the time.
Edit Encounter Details and Submit a New Claim
If you need to edit some aspect of the encounter and then optionally file a new claim, click "Edit Charges".
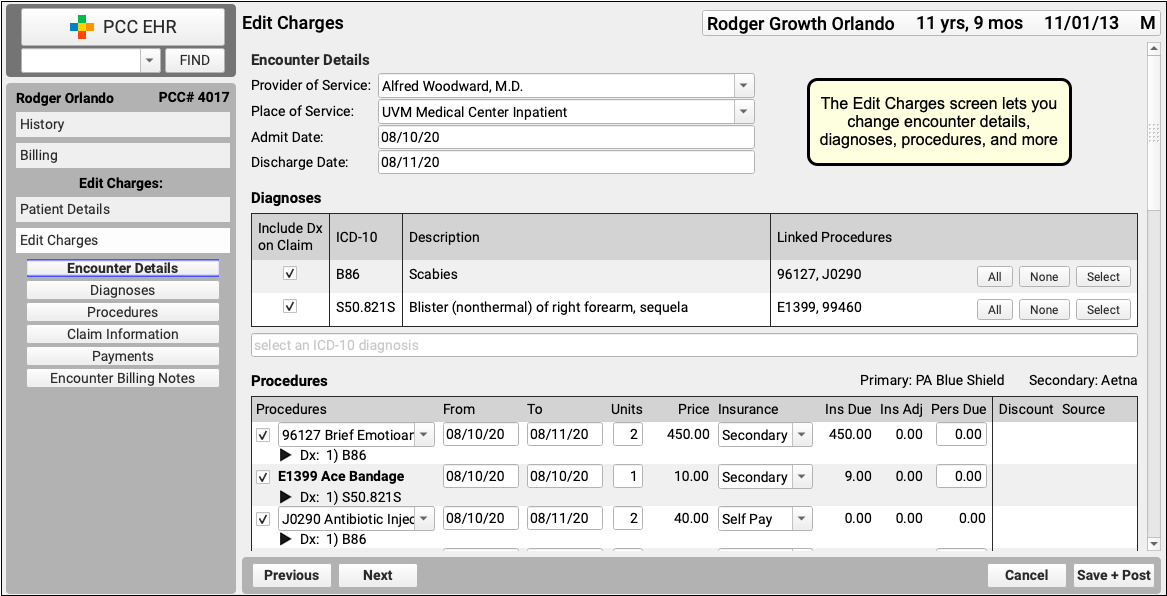
On the Edit Charges screen, you can change encounter details, diagnoses, procedures, and more.
If you need to file a corrected claim, you can review and adjust the responsible party for each charge, enter claim information, and queue up a new claim.
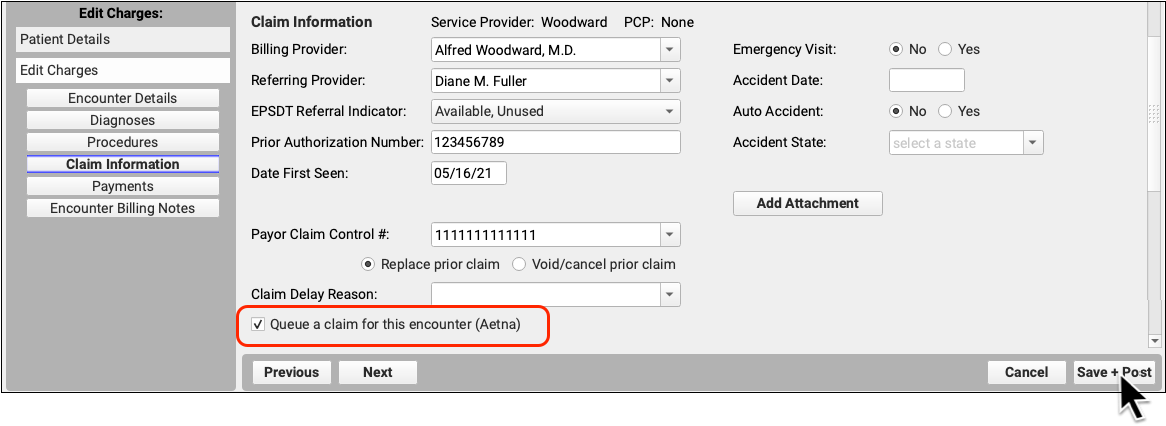
To learn more, read Edit Encounter Charges and Other Claim Information and Resubmit a Claim.
