Rejection and Unpaid Encounters Worklist Powers Snippet
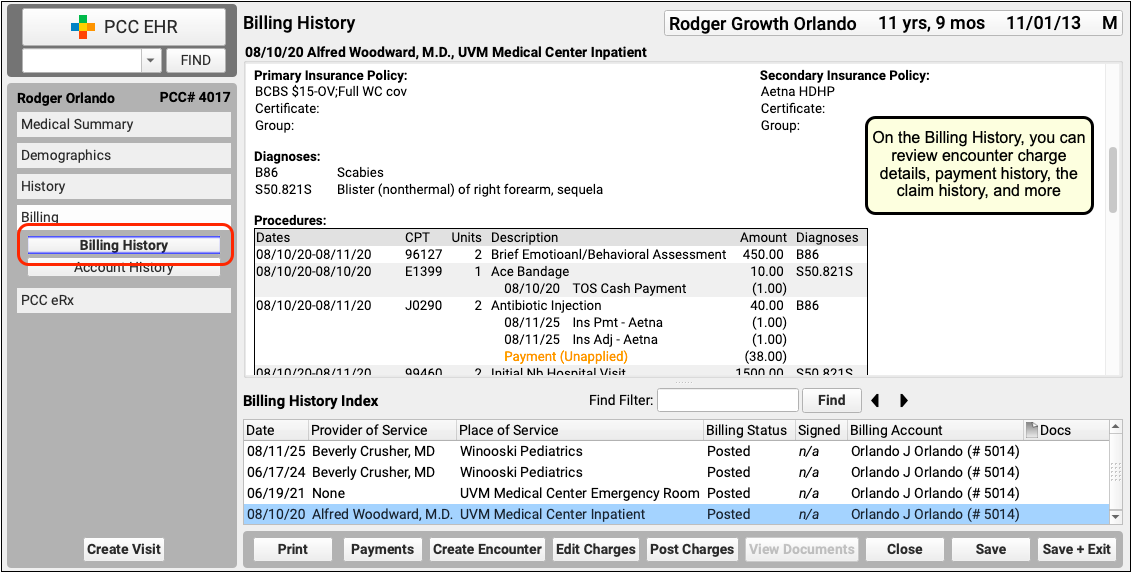
On the Billing History for the encounter, you can review full charge and payment details. The Claim History shows you all insurance billing activity and includes links to review the payor acknowledgements, posted ERAs, and more.
Review Patient Policies, the Complete Account History, and More
If you need to review more information about the patient and the account, you can navigate to other sections of the chart. For example, after clicking “Billing History”, click “Demographics” to review insurance policies.
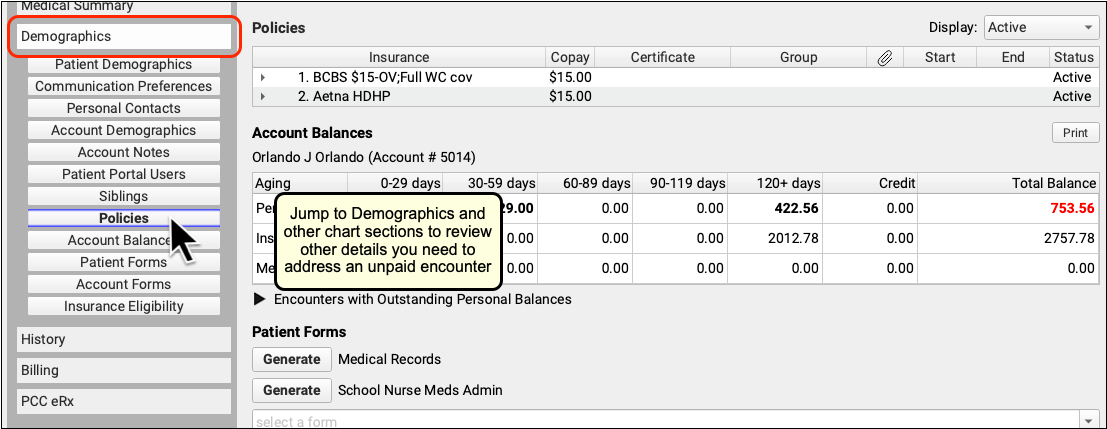
Or, to see the encounter and all financial transactions for the patient’s billing account, visit the Account History.
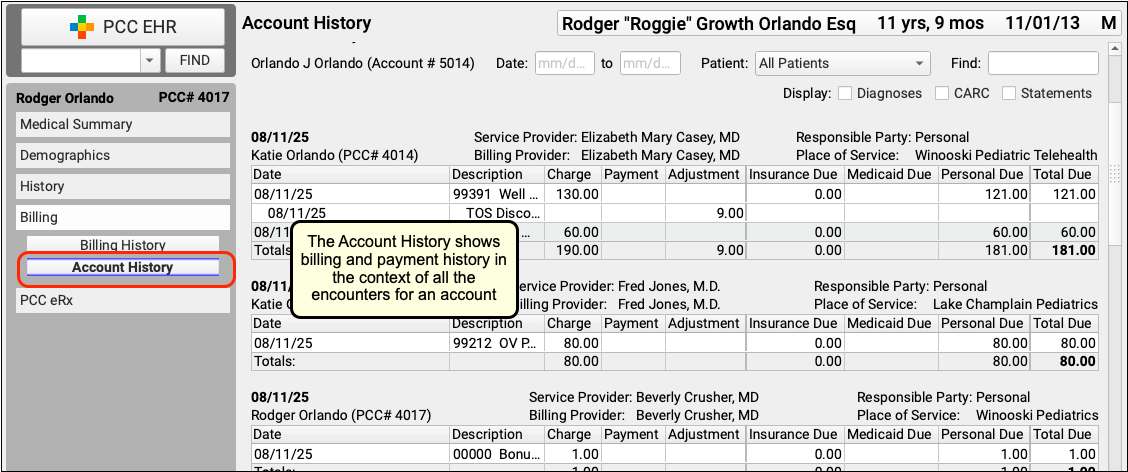
By reviewing the full account history, you can see every event linked to each encounter and also understand the encounter in the context of the family’s billing record.
Review Eligibility for the Encounter’s Date of Service
If you want to check if there are eligibility records for an encounter’s date of service, click “Edit Charges” and then “Patient Details” to see the eligibility component for that encounter.

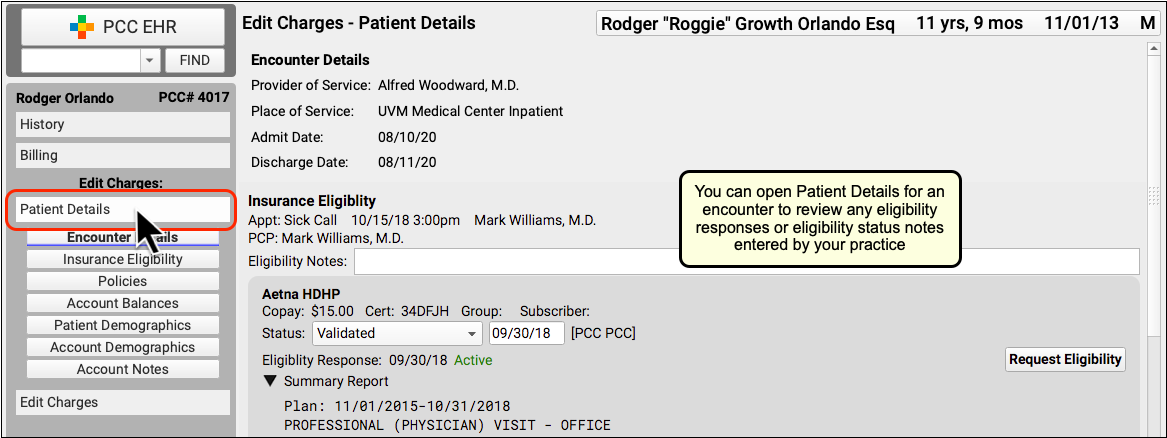
If your practice confirmed eligibility for the patient, either automatically or manually, you can review the results and any notes added at the time.
Edit Encounter Details and Submit a New Claim
If you need to edit some aspect of the encounter and then optionally file a new claim, click “Edit Charges”.
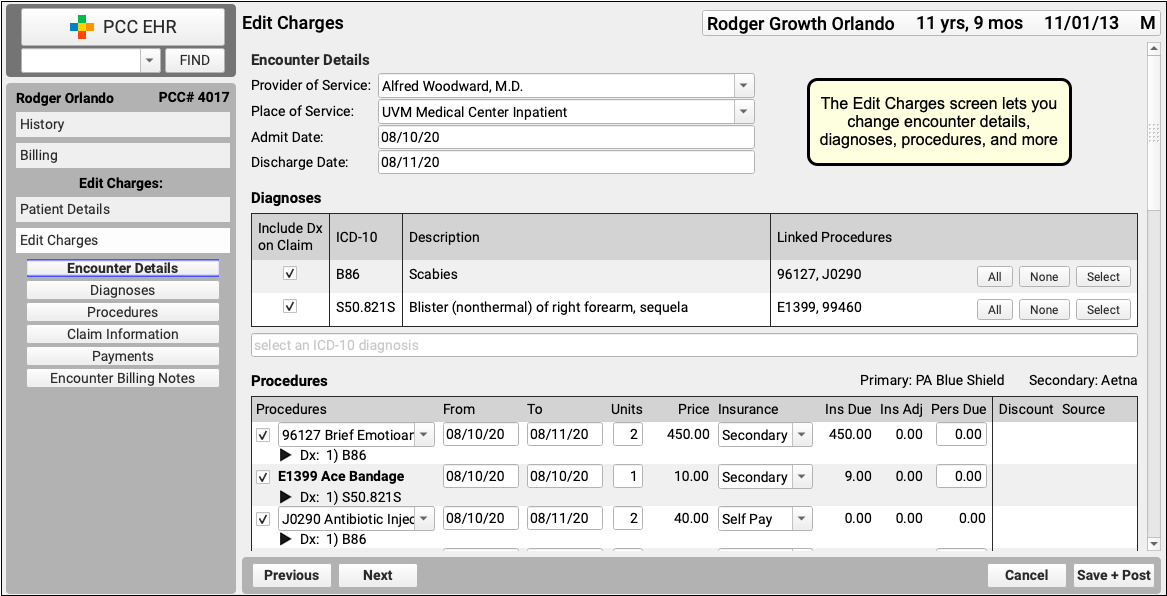
On the Edit Charges screen, you can change encounter details, diagnoses, procedures, and more.
If you need to file a corrected claim, you can review and adjust the responsible party for each charge, enter claim information, and queue up a new claim.
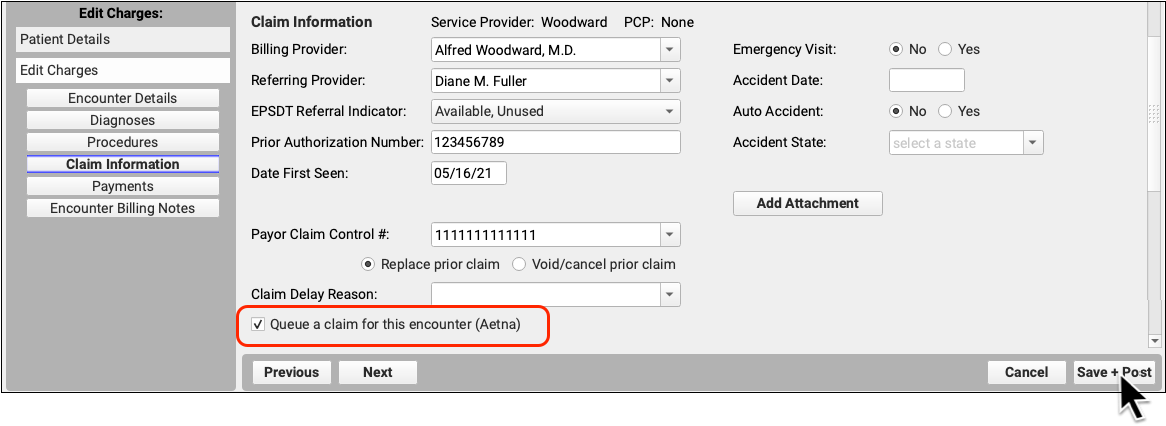
To learn more, read Edit Encounter Charges and Other Claim Information and Resubmit a Claim.
