How to Chart for Each Clinical Quality Measure in PCC EHR
You can use PCC EHR to collect data for the Clinical Quality Measures (CQMs) required by PCMH, the Medicaid EHR Incentive Program (“Meaningful Use”), and other mandate and pay-for-performance programs.
Read the article below to learn how to chart and configure your system in order to record medical information for each of 9 pediatric Clinical Quality Measures. By following these recommendations, and training your practice on charting workflow for CQMs, you can make sure that PCC EHR records the correct data to calculate your CQM performance.
Contents
- 1 Important Steps to Chart for Any CQM in PCC EHR
- 2 Pediatric CQMs Overview Chart: Adjust Your Practice’s Configuration and Visit Workflow
- 3 CMS2: Preventative Care and Screening: Screening for Clinical Depression and Follow-Up Plan
- 4 CMS75: Children Who Have Dental Decay or Cavities
- 5 CMS117: Childhood Immunization Status
- 6 CMS126: Use of Appropriate Medications for Asthma
- 7 CMS136: ADHD: Follow-up Care for Children Prescribed Attention Deficit/Hyperactivity Disorder (ADHD) Medication
- 8 CMS146: Appropriate Testing for Children with Pharyngitis
- 9 CMS153: Chlamydia Screening for Women
- 10 CMS154: Appropriate Treatment for Children with Upper Respiratory Infection (URI)
- 11 CMS155: Weight Assessment and Counseling for Nutrition and Physical Activity for Children and Adolescents
- 12 PCC’s Current Certification Status and Required CQMs for PCMH
- 13 What CQMs Are You Required to Report On
Important Steps to Chart for Any CQM in PCC EHR
The issues below affect every Clinical Quality Measure that PCC EHR measures, along with other reporting in PCC EHR.
Who is the Provider of Encounter?
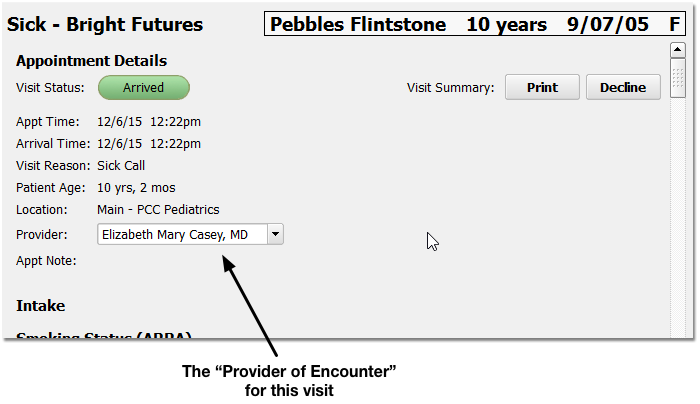
Clinical Quality Measures are calculated based on patient visits with specific eligible professionals, where the professional is the provider of encounter (PoE).
The PoE for a visit is listed at the top of every chart note. By default, it is defined when the visit is scheduled or when the chart note is created (for a walk-in visit). However, your practice can change the PoE when a different clinician sees the patient.
-
Check Your Practice Workflow: You should review your practice’s workflow to make sure that the provider at the top of the chart note is not changed for billing or patient management reasons. You should only change the provider of the encounter if a different clinician actually sees the patient.
-
Check Your Scheduling Providers: You should review your practice’s provider configuration to make sure the correct provider appears at the top of each chart note. For example, if you do not have a clinician listed correctly, or your practice schedules for a placeholder physician, you may want to review your configuration with PCC Support or review the steps in Add and Configure a Clinician.
-
Individual Clinicians vs. Practice Wide Reporting: As you review your list of providers, keep in mind that the EHR Medicaid Incentive Program (“Meaningful Use”) required CQM reporting individually, for each eligible professional. PCMH programs require CQM reporting in aggregate for your entire practice.
Know Which Codes (Value Sets) to Use for Each CQM
The NIH maintains a repository of codes used for public reporting purposes in its Value Set Authority Center (VSAC). The CMS eCQM Value Sets specify the various codes required for each Clinical Quality Measure.
For a few of the CQMs, PCC recommends using specific codes, such as when creating screening orders for depression. If this is the case, the recommended codes will be provided. Otherwise, links will be provided to the appropriate eCQM Value Set, on the VSAC website, and you can choose from the list of acceptable code(s) published for that data element.
Following is an example of a note from the ADHD Follow-up Care CQM section of this article:

You will need to have a username and password to access the eCQM Value Sets. It is a simple process to get access to the site; you will be directed to the application page from the login screen if you do not already have an account, or you can click here to request one.
It only takes a couple of minutes to fill out the request, and it generally takes only a day or two to receive your password.
What If I Don't Have Time/Don't Want a VSAC Account?: If you prefer not to setup and account on the VSAC website, or want access to the list of codes while you wait for your account to be approved, you can download the eCQM Value Sets spreadsheet and manually search for the list of codes you need. Each CQM has its own tab, and you can filter or sort by the “Value Set Name” column. The “Code” column displays the codes used within the measure.
Use Visit Codes to Record that a Visit Occurred
To correctly populate Clinical Quality Measures, your office should always use the “Bill” button, review the diagnoses and procedures for each visit, and select an appropriate visit code.
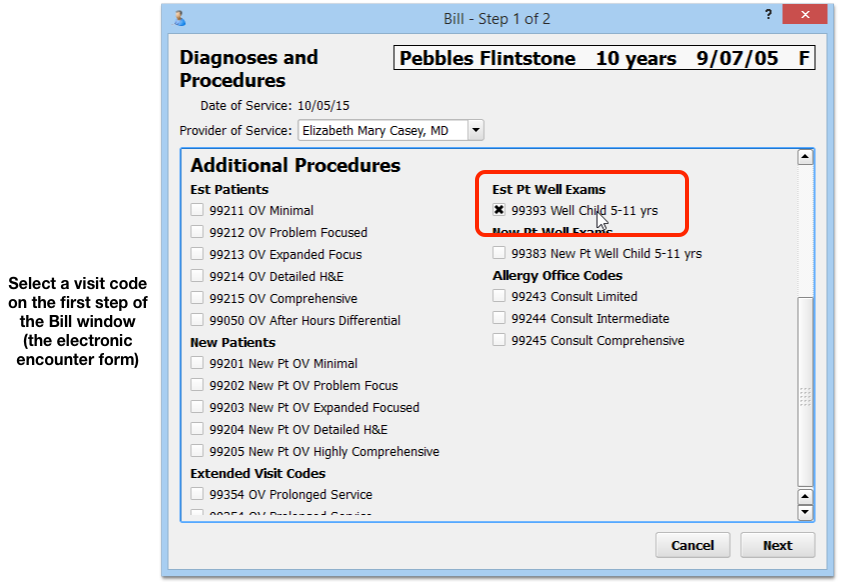
If your office does not use the electronic encounter form, contact PCC Support for help getting started.
What Visit Codes Should My Practice Use?: Valid encounter codes may vary from CQM to CQM, but generally include standard sick and well visits.
For example, the Childhood Immunization Status CQM calculation is based on patients who have an encounter code in one of the following Value Sets: “Office Visit”, “Face-to-Face Interaction”, “Home Healthcare Services”, “Preventative Care- Established Office Visit, 0 to 17”, and “Preventive Care- Initial Office Visit, 0 to 17”.
If you have questions about whether a specific SNOMED-CT, CPT, ICD-10, or other code meets the requirements for any CQM, you can reference the VSAC website. Alternatively, you can open the downloaded eCQM Value Sets spreadsheet, click on the tab for the appropriate CQM, and search/filter by the QDM Category “Encounter”.
How to Run the Clinical Quality Measures Report and See Your Practice’s Current Results
You can check your practice’s numbers for each CQM at any time.
The Clinical Quality Measures Report is available in the Reports menu in PCC EHR. Read the Run the Clinical Quality Measures Report article to learn how to run the report and e-mail the results.
Some of Your “Scores” May Be Low or May Be Zero
Clinical Quality Measures are designed to evaluate certain patient populations and compare chart activity to coding. You do not need to have a “high score” in order to qualify for the EHR Medicaid Incentive Program or to achieve PCMH recognition. The overall goal of CQM is to show improvement over time, and you can not show improvement for patient populations you do not serve.
It is important that you chart in such a way that the CQM tool can evaluate your score, but it is often not as important that you have a non-zero score. In fact, the new Dental Decay measure works in reverse, where decreasing your percentage over time is the goal. This is in contrast to the Meaningful Use Measures, for which your practice must meet certain threshold percentages in order to qualify for the ARRA incentive.
Pediatric CQMs Overview Chart: Adjust Your Practice’s Configuration and Visit Workflow
For a quick understanding of each measure, use the table below. You can click the “More Details” or “Show Me How” links to jump directly to a longer description, accompanied by screenshots and examples.
| CMS | NQF | Measure Name | Calculation Description | Configuration in PCC | Clinician Workflow |
|---|---|---|---|---|---|
| 2 | 0418 | Preventative Care and Screening: Screening for Clinical Depression and Follow-Up Plan | For all patients seen by the eligible professional during the reporting period, who were 12 years old or older before the beginning of the reporting period, who did not have a depression diagnosis or contraindication, who did not refuse the service, what percentage received a depression screening, and, if the result was positive, received additional followup care, such as a suicide risk assessment? (More Details) |
|
|
| 75 | N/A | Children Who Have Dental Decay or Cavities | For all patients seen by the eligible professional during the reporting period, who were between 0 and 20 years old, what percentage had tooth decay or cavities? (More Details) |
PCC EHR’s standard installation includes all of the configuration required in order to chart for this measure. Optionally, your practice can edit your chart note protocols to make it easier to record dental health and/or order followup dental care. |
|
| 117 | 0038 | Childhood Immunization Status | For all patients seen by the eligible professional during the reporting period and turning 2 years old during the reporting period, what percentage had four diphtheria, tetanus and acellular pertussis (DTaP); three polio (IPV), one measles, mumps and rubella (MMR); three H influenza type B (HiB); three hepatitis B (Hep B); one chicken pox (VZV); four pneumococcal conjugate (PCV); one hepatitis A (Hep A); two or three rotavirus (RV); and two influenza (flu) vaccines by their second birthday, or had a documented history of the illness, seropositive result for the antigen, or a contraindication for a specific immunization? (More Details) |
PCC EHR’s standard installation includes most of the configuration required in order to chart for this measure.
|
|
| 126 | 0036 | Use of Appropriate Medications for Asthma | For all patients seen by the eligible professional during the reporting period, who were between 5 and 64 years old, and have an active, persistent asthma diagnosis during the reporting period, what percentage were prescribed or had an active prescription for an appropriate medication? (More Details) |
PCC EHR’s standard installation includes all of the configuration required in order to chart for this measure. |
|
| 136 | 0108 | ADHD: Follow-up Care for Children Prescribed Attention Deficit/Hyperactivity Disorder (ADHD) Medication | For all patients who were newly dispensed a medication for attention-deficit/hyperactivity disorder (ADHD) during the reporting period, who were between 6 and 12 years old, what percentage had appropriate followup care, including a follow-up visit with a practitioner with prescribing authority during the 30-Day Initiation Phase, and, if remaining on the medication for at least 210 days, had at least two additional follow-up visits with a practitioner within 270 days (9 months) after the Initiation Phase ended? (More Details) |
PCC EHR’s standard installation includes all of the configuration required in order to chart for this measure. Optionally, your practice can maintain an ADHD-specific chart note protocol, and include follow-up visit orders within that protocol. (Show Me How) |
|
| 146 | 0002 | Appropriate Testing for Children with Pharyngitis | For all patients seen by the eligible professional during the reporting period, who were between 2 and 18 years old, who were diagnosed with pharyngitis during the reporting period, who were prescribed an antibiotic within three days of an encounter, for what percentage of those encounters did patients receive a group A streptococcus (strep) test? (More Details) |
PCC EHR’s standard installation includes all of the configuration required in order to chart for this measure. You may want to review your order configuration for group A streptococcus (Rapid Strep) orders, and/or edit your chart note protocols to make it easier to diagnose pharyngitis and create orders. (Show Me How) |
|
| 153 | 0033 | Chlamydia Screening for Women (Summary) | For all female patients seen by the eligible professional during the reporting period, who were between 16 and 24 years old, who were sexually active, what percentage had at least one chlamydia test during the reporting period? (More Details) |
|
|
| 154 | 0069 | Appropriate Treatment for Children with Upper Respiratory Infection (URI) | For all patients seen by the eligible professional during the reporting period, who were between 3 months and 18 years of age, who were diagnosed with an upper respiratory infection, what percentage were not dispensed an antibiotic prescription on or three days after the episode? (More Details) |
PCC EHR’s standard installation includes all of the configuration required in order to chart for this measure. You may want to edit your chart note protocols to make it easier to diagnose URI. (Show Me How) |
|
| 155 | 0024 | Weight Assessment and Counseling for Nutrition and Physical Activity for Children and Adolescents | For all patients seen by the eligible professional during the reporting period, who were between 3 and 17 years of age, what percentage had their height, weight, and BMI recorded, and what percentage received counseling for nutrition and/or physical activity? (More Details) |
|
|
CMS2: Preventative Care and Screening: Screening for Clinical Depression and Follow-Up Plan
This measure calculates the percentage of patients aged 12 years and older who are screened for clinical depression on the date of their encounter using an age-appropriate standardized depression screening tool AND if positive, a follow-up plan is documented on the date of the positive screen. (CMS at eCQI)
-
Denominator: PCC EHR calculates the denominator of this measure by counting all patients who had an eligible encounter code billed in the electronic encounter form during the reporting period and who were 12 or older before the reporting period.
-
Numerator: PCC EHR calculates the numerator of this measure by counting all of the patients in the denominator who had a LOINC test for depression screening, generally inside a Depression Screening order, with a positive or negative result, on the encounter date. If the result was positive, the patient must have additional care in the form of a completed LOINC test for suicide risk assessment, follow-up or additional evaluation for depression, and/or a referral for depression, and/or a prescription for a depression medication, on the same date as the depression screening, in order to be included in the numerator.
-
Exclusions: If a patient had an active diagnosis for Depression or Bipolar Disorder on their Problem List or in the Diagnoses component for the visit, they will be counted in the Exclusions for the measure.
-
Exceptions: If a patient refused the screening, or had a medical contraindication for it being performed, such as an urgent medical situation or a lack of functional capacity to complete the screening, they are excepted from the denominator (and the numerator) for the calculation and will be counted in the Exceptions for the measure.
Recommended PCC EHR Configuration for CMS2 Depression Screening
In order to chart depression screenings, followup, and suicide risk assessment, your practice can create screening orders and add the specified LOINC tests or SNOMED-CT descriptions to those orders. You can also configure referral orders so that they are recorded with an appropriate SNOMED-CT. Finally, you can add the orders to chart notes so they are easy to select at every visit.
For a step-by-step procedure on how to add codes to orders and add specific orders to chart notes, read Use Orders to Track Measures for Mandates.
Configure Your Depression Screenings
Add SNOMED-CT and LOINC codes to your adolescent depression screening orders in PCC EHR.
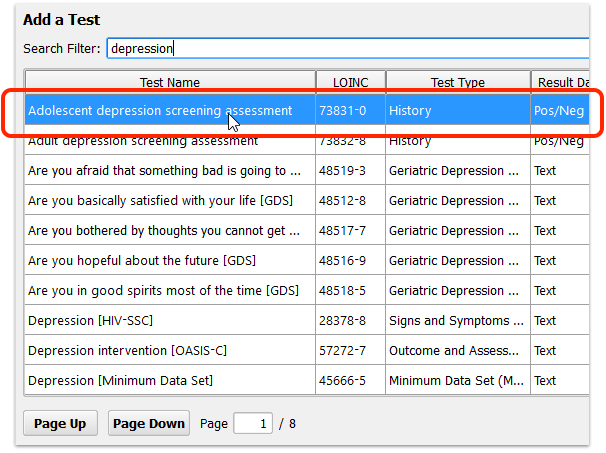
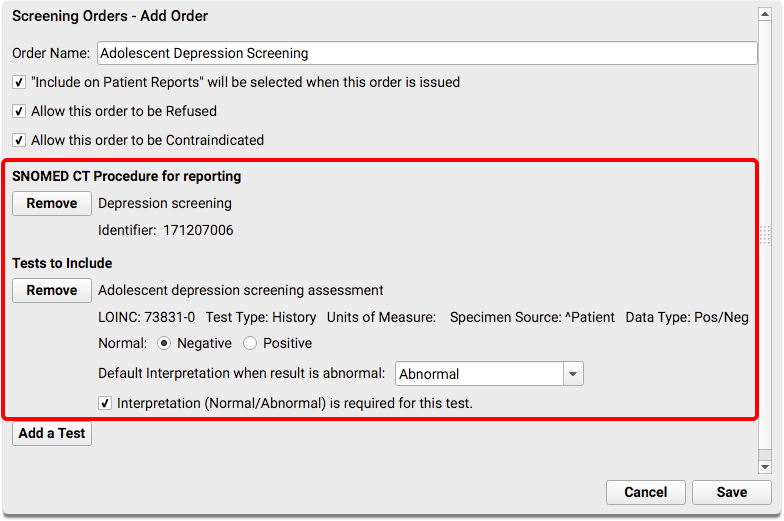
For the initial depression screening, you should add SNOMED-CT procedure code 171207006, and LOINC test code 73831-0, “Adolescent depression screening assessment”. (You could also add LOINC 73832-8, “Adult depression screening assessment” for an order for patients 18 years or older.) The test should have a Negative/Positive result.
What About Other Depression Screening Tests?: Your practice might perform other depression screenings and use other LOINC tests to record discrete results. You can add more than one test to a single order. For example, if you perform a PHQ-9 at each visit, you might first add the “Adolescent depression screening assessment” test, which is used by the clinical quality measure, and then also add the “Patient Health Questionnaire 9 item (PHQ-9) total score” test in order to record the patient’s numerical result.
Configure Followup Depression Care
When a patient has a positive result on a depression screening, your practice might perform one or more additional evaluations, followup orders, or a suicide risk assessment screening order. Click “Add” to create a new screening order, or double-click on an existing order to make changes. Repeat the steps above to configure the order, and add any appropriate tests.
In order to affect the clinical quality measure for this additional evaluation, followup, or suicide risk assessment, your practice must also add SNOMED-CT procedures to the screening order. For each order, click “Add a Procedure” and search for the appropriate SNOMED-CT description.
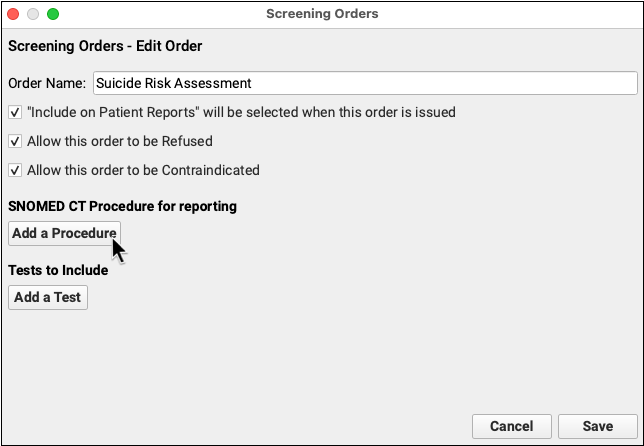
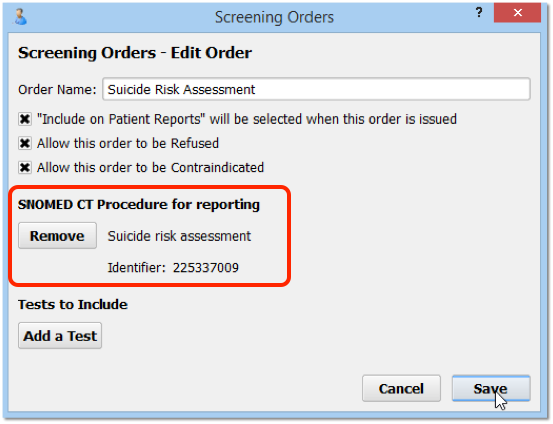
Examples:
-
Suicide Risk Assessment: For a suicide risk assessment screening order, you should add SNOMED-CT code 225337009, “Suicide risk assessment (procedure)” to the order.
-
Followup For Depression: You could also create and add SNOMED-CT descriptions (and LOINC tests, if appropriate) for any number of depression followup orders, such as Completion of a Mental Health Crisis Plan, or Coping Support Management. Other options are included in the NIH’s Follow-up for depression – adolescent value set, found on the VSAC website. You can also find the “Follow-up for depression – adolescent” value set within the CMS2v4 tab of the downloaded eCQM Value Sets spreadsheet.
-
Additional Evaluation: For an additional evaluation for depression order, you could add one of the SNOMED-CT descriptions for psychiatric evaluation listed by NIH for Additional evaluation for depression – adolescent. The “Additional evaluation for depression – adolescent” value set can also be found within the CMS2v4 tab of the downloaded eCQM Value Sets spreadsheet.
Configure Depression Referral Orders
Add SNOMED-CT procedures to your Referral orders for Depression.
Your practice may have one or more referrals related to depression. For example, you may have referrals for an initial psychiatric evaluation or a specific depression referral. Click “Add” to create a new order, or double-click on an existing order to make changes.
In order for the referral to be tracked as part of a clinical quality measure, you must add a SNOMED-CT description from the NIH’s list for “Referral for Depression Adolescent”.
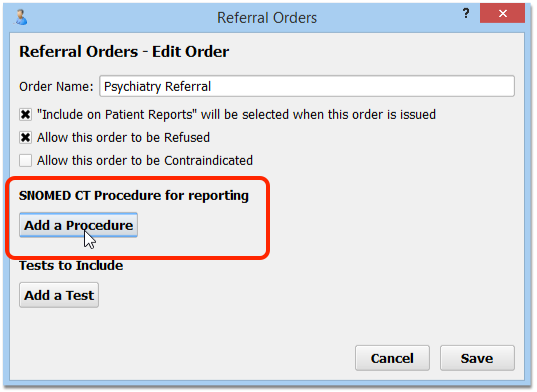
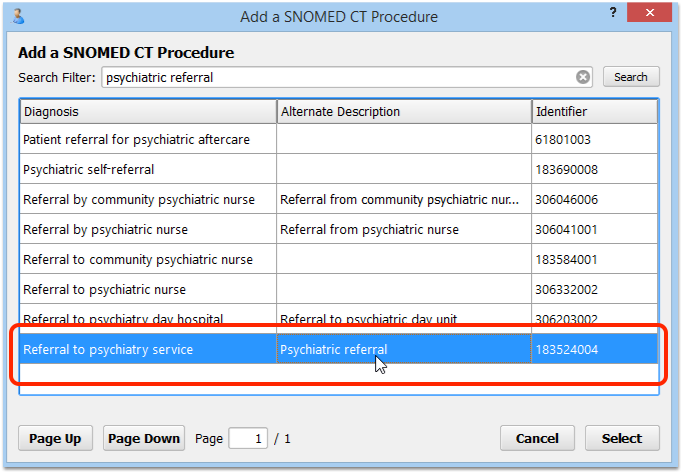
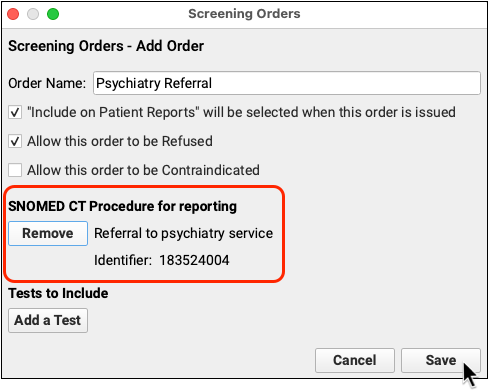
Which Procedure Codes Can I Use for Referral Orders?: Your SNOMED-CT descriptions for depression-related referrals must be taken from the NIH’s Referral for Depression Adolescent value set, found on the VSAC website. Common selections include “Referral to psychiatry service” and “Referral for mental health counseling”. You can also find the “Referral for Depression Adolescent” value set within the CMS2v4 tab of the downloaded eCQM Value Sets spreadsheet.
Your practice may have other referrals that may follow a positive depression screening. Add new orders, or double-click on an existing order to make changes.
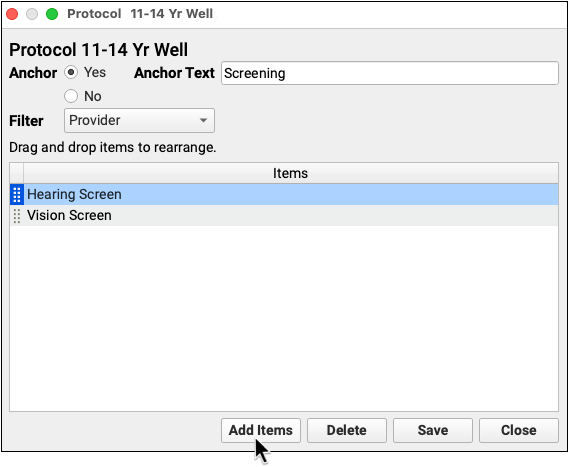
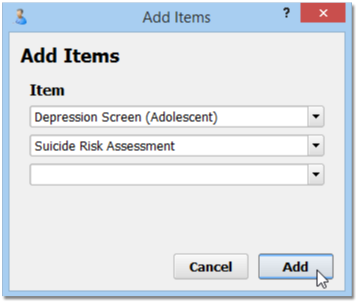
Add Depression Screening, Suicide Risk Assessment, and Referral Orders to Your Chart Note Protocols
After you make changes to the various orders your practice uses, you can add them to chart note protocols to make them easier to order. Your clinicians will then see the “Depression Screening” order, for example, on every chart note.
For information on how to add specific orders to a chart note protocol, read Use Orders to Track Measures for Mandates.
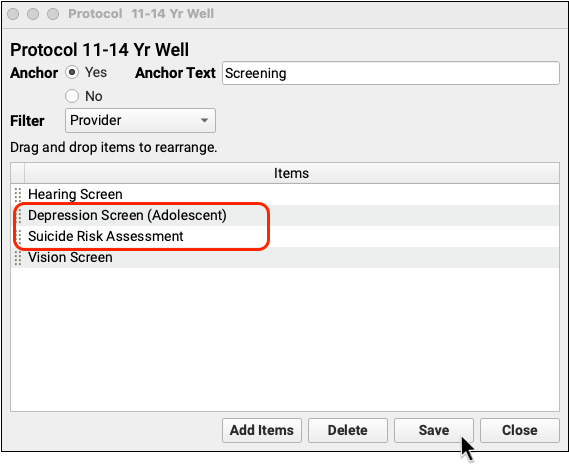
Recommended Charting and Workflow for CMS2 Depression Screening
When a patient twelve or older visits your practice, click “Order” to order a Depression Screening.
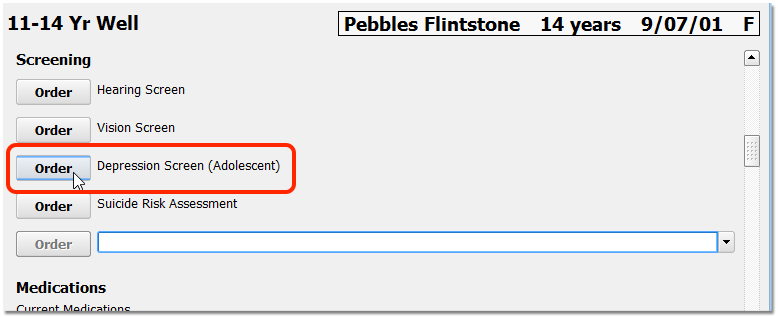
Optionally, you can assign the screening to another clinician, or complete the screening immediately. If the screening is refused, select “Refused”. If the screening is contraindicated, select “Contraindicated” and enter an appropriate contraindicated diagnosis in the Diagnoses component on the chart note.
When the screening is complete, enter a result.
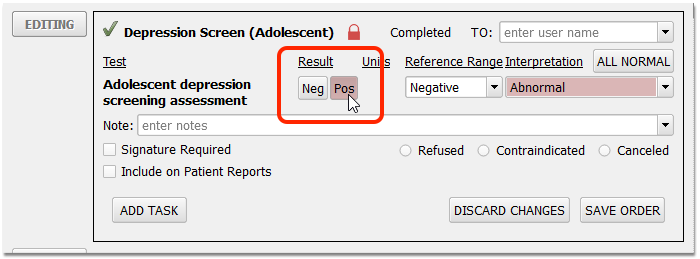
Unless refused or contraindicated, a positive or negative result is required. Result interpretation, in the Interpretation field, is not required for the clinical quality measure, though your practice may have configured it to be required for completion of the order.
If the result is positive, record whatever additional care follows.
For example, you may prescribe appropriate medication, order a Suicide Risk Assessment or order a referral.
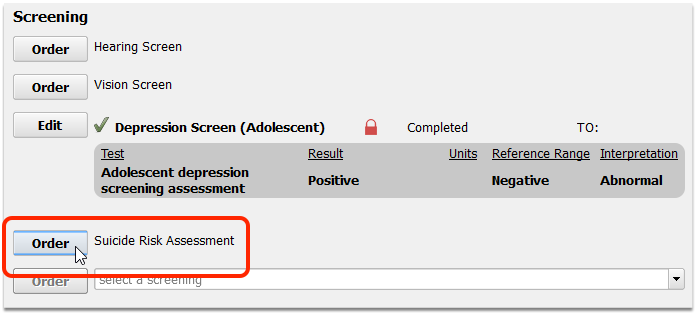
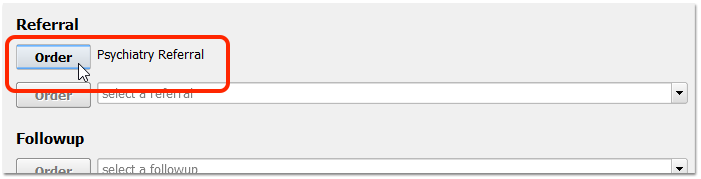
Enter results and take any other appropriate followup steps.
When you are finished charting, remember to click “Bill” and select an appropriate visit encounter code. In addition to billing, the visit encounter code is used to calculate the CQM.
CMS75: Children Who Have Dental Decay or Cavities
This measure calculates the percentage of patients aged 0-20 who have a visit during the reporting period and have an active diagnosis of tooth decay or cavities during the measurement period. (CMS at eCQI)
-
Denominator: PCC EHR calculates the denominator of this measure by counting all patients who had an eligible encounter code billed on the electronic encounter form during the reporting period and who were between 0 and 20 years old.
-
Numerator: PCC EHR calculates the numerator of this measure by counting all of the patients in the denominator who had a dental decay or cavity diagnosis in the Diagnoses component for a visit during the reporting period or an active dental decay or cavity diagnosis listed in their Problem List.
-
Exclusions: There are no exclusions for this measure. All patients can qualify for the numerator.
-
Exceptions: There are no exceptions for this measure. All patients can qualify for the denominator.
Recommended PCC EHR Configuration for CMS75 Dental Decay
There are no recommended PCC EHR configuration changes for recording data that will affect the dental decay clinical quality measure.
Your practice may want to review your chart note protocols and make adjustments for recording dental health. For example, your physical exam component may benefit from a “Teeth (caries, white spots, staining)” or “Dental Health” item. Your practice may want to add other items to chart note protocols, such as a “Child has a dental home” option in the History component, which is a recommendation in the AAP’s Bright Futures materials. However, those changes will not affect this clinical quality measure.
If your practice administers fluoride varnish or does dental evaluations, you may want to review your chart note protocols and create and add appropriate orders to your chart notes. However, those changes will not affect this clinical quality measure.
Recommended Charting and Workflow for CMS75 Dental Decay
When a patient visits your practice, evaluate and chart their dental health.
Optionally, you might record details in one or more components on the chart note.
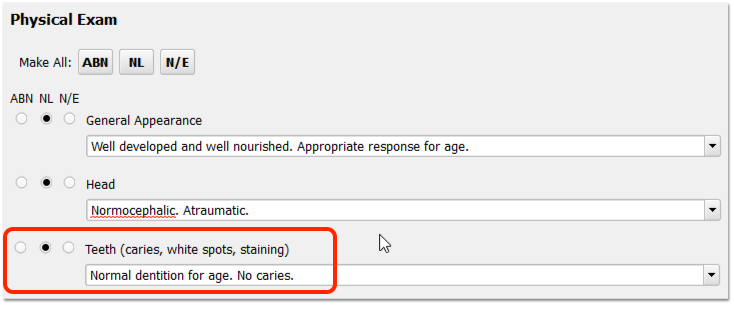
If the patient has tooth decay or cavities, enter an appropriate diagnosis code in the Diagnoses component.
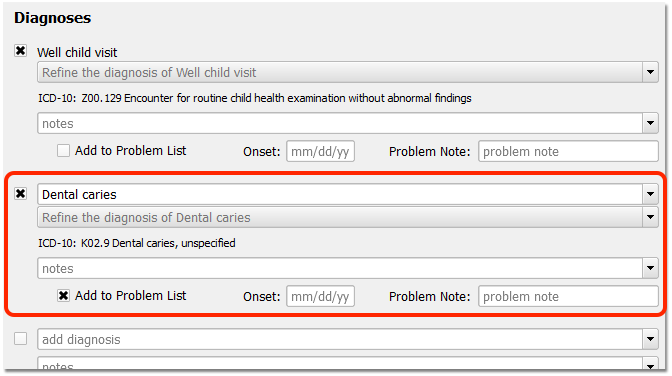
Which Diagnoses Should I Use for Dental Decay?: The NIH lists several acceptable SNOMED-CT diagnosis descriptions in the “Dental Caries Grouping Value Set” (2.16.840.1.113883.3.464.1003.125.12.1004). Diagnoses range from “Dental caries” to “Secondary dental caries associated with failed or defective dental restoration”.
Optionally, you might order and perform additional evaluations or treatment, or provide educational materials. Those actions do not affect this clinical quality measure.
When you are finished charting, remember to click “Bill” and select an appropriate visit encounter code. In addition to billing, the visit encounter code is used to calculate the CQM.
CMS117: Childhood Immunization Status
This measure calculates the percentage of patients turning 2 years old during the reporting period who have a visit during the reporting period and have four diphtheria, tetanus and acellular pertussis (DTaP); three polio (IPV), one measles, mumps and rubella (MMR); three H influenza type B (HiB); three hepatitis B (Hep B); one chicken pox (VZV); four pneumococcal conjugate (PCV); one hepatitis A (Hep A); two or three rotavirus (RV); and two influenza (flu) vaccines with evidence of administration prior or on their second birthday. (CMS at eCQI)
-
Denominator: PCC EHR calculates the denominator of this measure by counting all patients who turned 2 years old during the reporting period, who had an eligible encounter code entered on the electronic encounter form during the reporting period.
-
Numerator: PCC EHR calculates the numerator of this measure by counting all of the patients in the denominator who have evidence of meeting all the immunization requirements, either ordered, added manually to the patient record, or billed. In order to allow for “grace periods”, the timing requirements for each immunization (three shots, four shots, etc.) require a minimum of only a single day between each shot, and allow that the shots may occur at any time between birth and age 2 after each shot’s minimum age. For example, a patient’s first DTaP must be administered when the patient is at least 42 days old, but otherwise the four shots may occur at any time before or on the patient’s 2nd birthday, as long as they are at least a day apart.
-
Exclusions and Exceptions: There are no across-the-board exclusions or exceptions for this measure. However, there are numerous reasons that a patient may be included in the numerator even if they did not have a particular shot.
For the MMR, hepatitis B, VZV and hepatitis A vaccines, numerator inclusion criteria include: evidence of receipt of the recommended vaccine; documented history of the illness; or, a seropositive test result for the antigen. For the DTaP, IPV, HiB, pneumococcal conjugate, rotavirus, and influenza vaccines, numerator inclusion criteria include only evidence of receipt of the recommended vaccine. Patients may be included in the numerator for a particular antigen if they had an anaphylactic reaction to the vaccine. Patients may be included in the numerator for the DTaP vaccine if they have encephalopathy. Patients may be included in the numerator for the IPV vaccine if they have had an anaphylactic reaction to streptomycin, polymyxin B, or neomycin. Patients may be included in the numerator for the influenza, MMR, or VZV vaccines if they have cancer of lymphoreticular or histiocytic tissue, multiple myeloma, leukemia, have had an anaphylactic reaction to neomycin, have Immunodefiency, or have HIV. Patients may be included in the numerator for the hepatitis B vaccine if they have had an anaphylactic reaction to common baker’s yeast.
The measure allows a grace period by measuring compliance with these recommendations between birth and age two. (From the “Guidance” section of CMS’s definition of the CQM.)
For the above exclusions, PCC checks the patient’s diagnosis history, Problem List, and Allergies List.
Recommended PCC EHR Configuration for CMS117 Childhood Immunization Status
When your practice implemented PCC software and services, the initial setup and configuration was sufficient to allow clinicians to chart in order to meet this CQM.
However, if your practice implemented PCC software before the introduction of CVX codes, which are used to uniquely identify immunizations, you need to add them to your Immunization and Disease table in the Table Editor (ted).
You may also want to review your chart note protocols so that every clinician can quickly and easily order age-appropriate immunizations for each patient.
Review and Update Your Practice's CVX Code Configuration For Each Immunization You Record, Administer, or Bill
CVX codes are the industry-standard unique identifier for each vaccine or combination vaccine. Follow the procedure below to update your immunizations with CVX codes.
Open the Table Editor (ted)
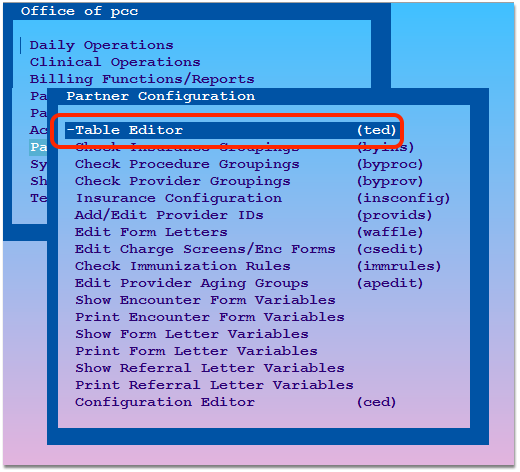
Open the Immunization and Disease Table
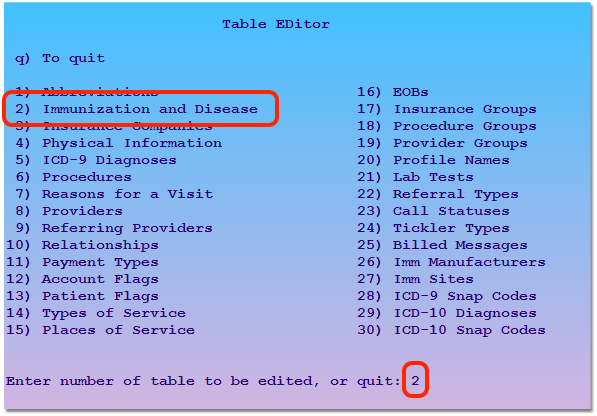
Open the First Immunization You Record, Administer, or Bill
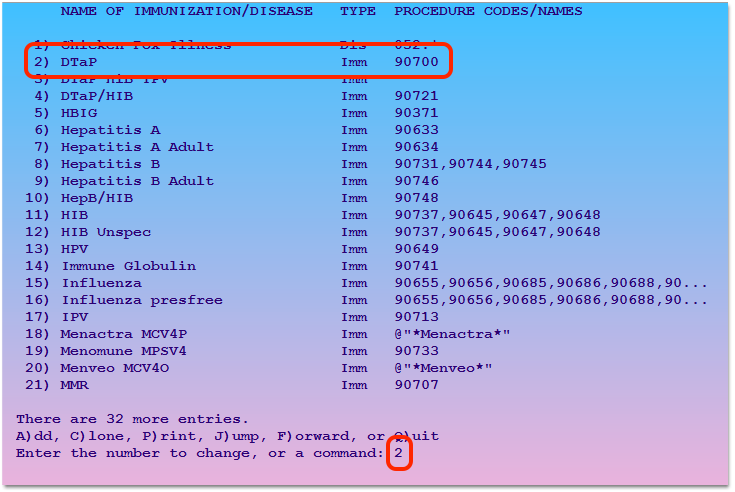
Update It With the Correct CVX Code
Enter the CVX code in the “CVX Code” field.
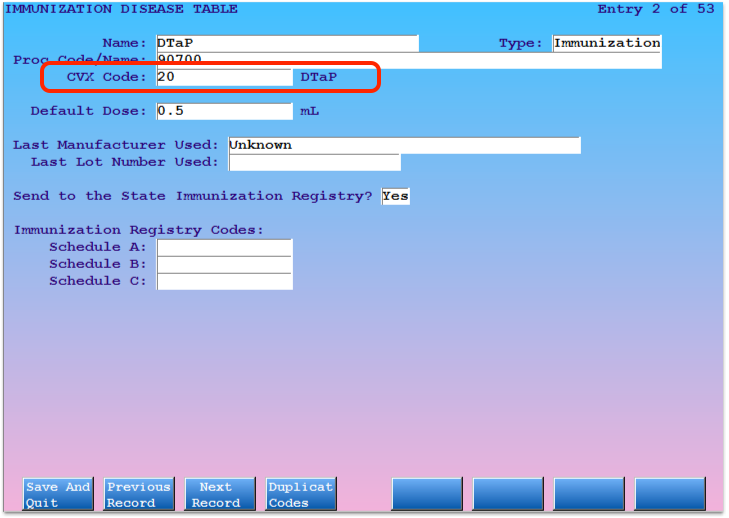
What CVX Code Should I Use?: Different combination vaccines and different formulations have different CVX codes. The only way to be certain you are selecting the correct code is to visit your immunization refrigerator, and optionally use PCC’s cvxreport to compare your practice’s configuration with the CDC’s library of CVX codes. However, the some common CVX codes for each immunization are as follows: DTaP 20, IPV 10, MMR 03, HIB 49, Hepatitis B 08, Varicella (chicken pox) 21, Prevnar 13 (pneumococcal conjugate PCV) 133, Hepatitis A 83, Rotavirus 116, Influenza (Flu) Preservative Free 140.
Repeat the Above Steps for Each Immunization You Administer or Record in a Patient’s Chart
Whether you order and administer an immunization or combination vaccine, or only need to be able to record it in a patient’s history, enter the appropriate CVX code for each entry.
If an immunization is missing, review the steps in the Add and Configure an Immunization in PCC EHR and Partner help article.
Review Your Entire CVX Code Configuration and Compare it With All CDC Codes
Optionally, your practice can run PCC’s cvxreport program to review all your CVX codes and compare them with the national code list.
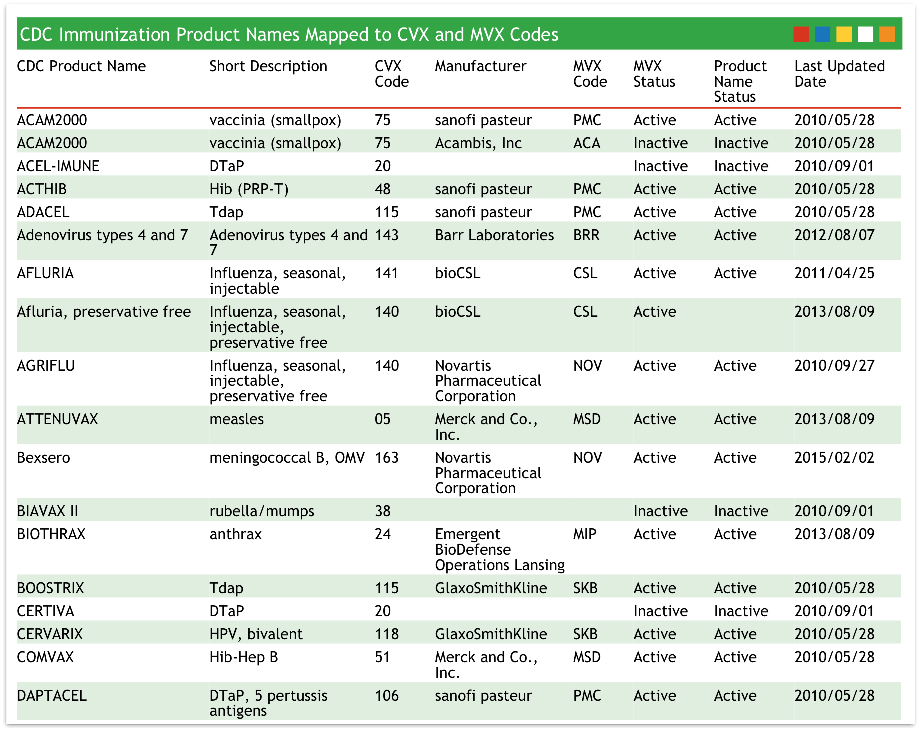
Add Age-Appropriate Immunizations to Your Custom Chart Notes
Do all of your custom chart notes have age-appropriate immunization orders ready, easy for your clinicians to click?
If not, follow the procedure below to update your chart note protocols.
Add Age-Appropriate Immunizations to Your Custom Chart Notes
Recommended Charting and Workflow for CMS117 Childhood Immunization Status
When a patient visits your practice, review their immunization history in the chart note or in the Immunization History section of the chart.
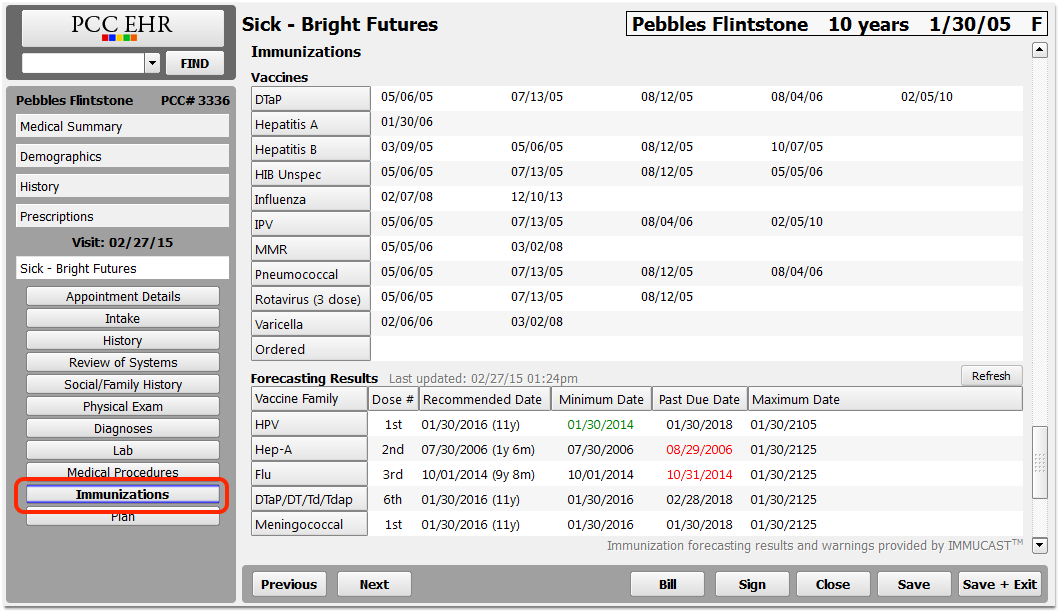
Optionally, you can review Forecasting Results and Forecasting Warnings to see what immunizations a patient may be missing.
If you need to update a patient’s past immunization history, visit the Immunization History section of the chart, click “Add Imms” and add any immunizations they received that are not in the chart record.
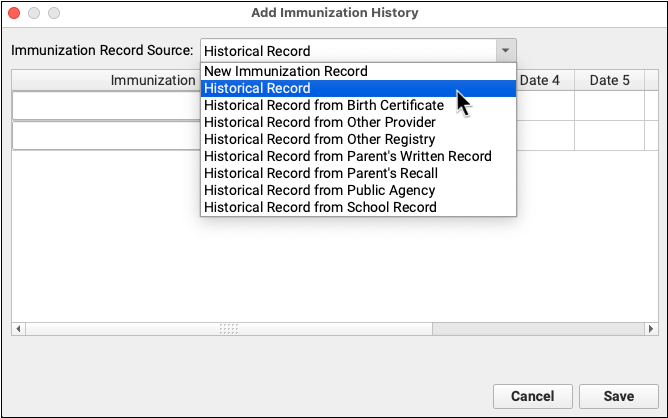
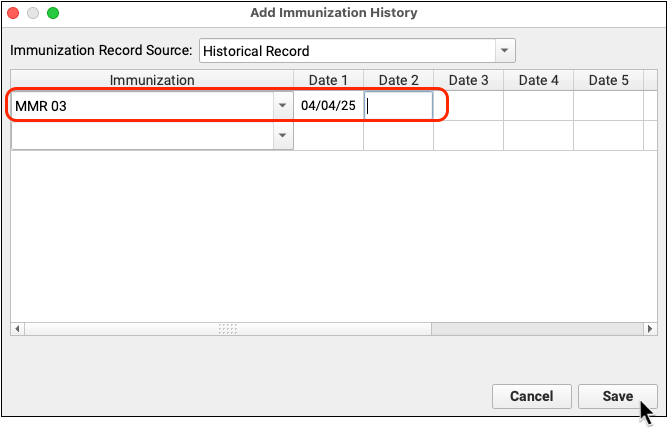
Use the Immunizations component on the chart note to order any age-appropriate immunizations.
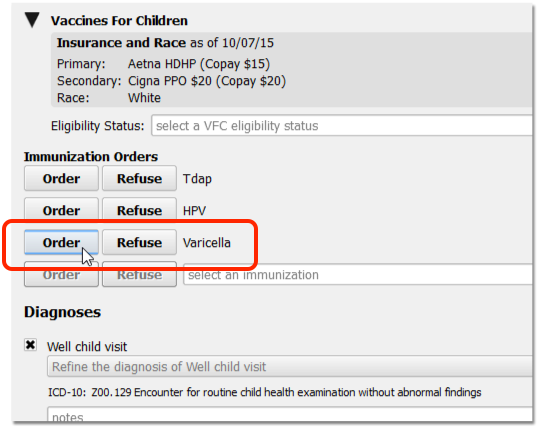
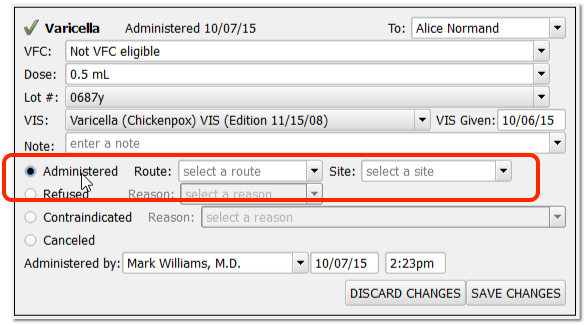
Use the same component (or “Edit Orders” orange indicator tool on Schedule screen) to record that the immunization is administered, refused, contraindicated, or canceled.
When Should Each Shot Be Given?: PCC EHR can display Immunization Forecasting, with results and forecasting calculated by STC’s implementation of the ACIP immunization schedule guidelines from the CDC. Your practice may have their own set of standards for how these guidelines are implemented, and CMS has their own published clinical recommendation based on ACIP’s guidelines. The rules for reporting for the Childhood Immunization Status CQM, however, are much simpler, only requiring the correct number of shots, given more than a day apart.
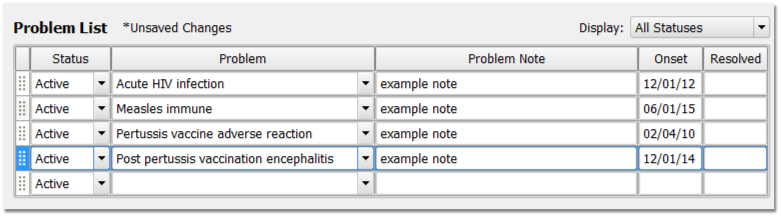
If you make a decision not to give an immunization, chart the reason in the following manner:
-
Contraindications: If a patient has a contraindication for an immunization, click “Contraindicated” in the order, and add the appropriate diagnosis description to the Diagnoses component in the chart note and/or to the patient’s Problem List or Allergies list. For example, if a patient has acute HIV infection, or an allergy to an immunization component, you should record that information in the Problem List and the Allergies List respectively.
-
History of an Illness: If a patient has a history of an illness for which an immunization would otherwise be administered, add that illness to the patient’s Problem List or chart it in the Diagnoses component.
-
Evidence of Immunity: If your practice performs titers, or receives a test result showing that the patient is seropositive for an antigen, record that result as a diagnosis or on the Problem List.
When you are finished charting, remember to click “Bill” and select an appropriate visit encounter code. In addition to billing, the visit encounter code is used to calculate the CQM.
CMS126: Use of Appropriate Medications for Asthma
This measure calculates the percentage of patients 5-64 years of age who were identified as having persistent asthma and were appropriately prescribed medication during the measurement period. (CMS at eCQI)
-
Denominator: PCC EHR calculates the denominator of this measure by counting all patients who had an eligible encounter code billed on the electronic encounter form during the reporting period, who were between 5 and 64 years old, who had a diagnosis of persistent asthma.
-
Numerator: PCC EHR calculates the numerator of this measure by counting all of the patients in the denominator who were dispensed at least one prescription for a preferred therapy during the measurement period or had an active medication listed during the measurement period.
-
Exclusions and Exceptions: Patients will be excluded from the denominator if they have a diagnosis of emphysema, COPD, cystic fibrosis or acute respiratory failure during or prior to the measurement period.
Recommended PCC EHR Configuration for CMS126 Use of Appropriate Medications for Asthma
There are no required PCC EHR configuration changes for recording data that will affect the Appropriate Medications for Asthma CQM.
Your practice may want to review your chart note protocols and make adjustments for reviewing medication history for a patient. For example, you could add the Medication History component to chart notes, or add a “Reviewed Medications” checkbox.
Your practice or clinicians may want to review your prescription Favorites lists, found in PCC eRx, the prescription module in PCC EHR. For example, you could add common asthma medications to the list.
Recommended Charting and Workflow for CMS126 Use of Appropriate Medications for Asthma
When a patient visits your practice, chart any appropriate asthma diagnoses in the Diagnoses component and/or the patient’s Problem List.
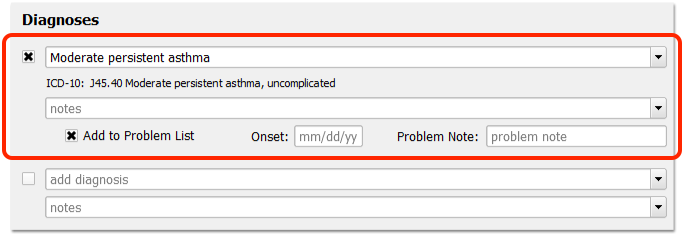
When a patient has a diagnosis of persistent asthma, use the Prescriptions section of the chart to prescribe appropriate medications.
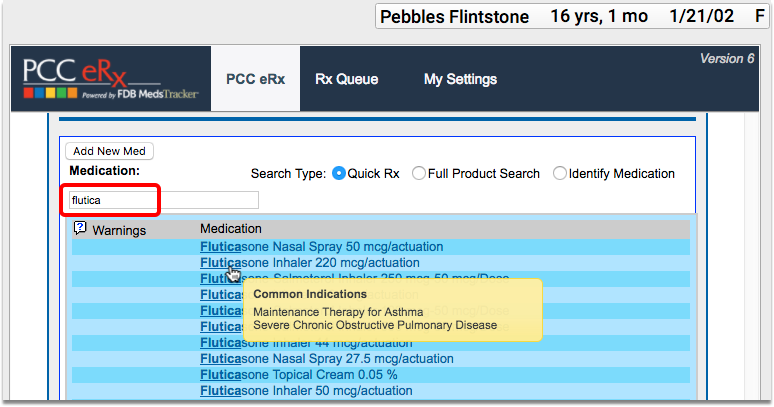
What Specific Diagnoses Count as Persistent Asthma for this CQM?: The four SNOMED-CT descriptions that are considered persistent asthma by CMS are Persistent asthma, Mild persistent asthma, Moderate persistent asthma, and Severe persistent asthma. There are additional ICD-10 billing codes, which are included in the NIH’s Persistent Asthma value set, found on the Value Set Authority Center website. You can also find the “Persistent Asthma” value set within the CMS126v3 tab of the downloaded eCQM Value Sets spreadsheet.
What Are Appropriate Medications for Persistent Asthma for This CQM?: The NIH includes a number of medications in its Preferred Asthma Therapy value set, including common medications such as fluticasone, cromolyn, salmeterol and fluticasone combinations, theophylline, etc. You can also find the “Preferred Asthma Therapy” value set within the CMS126v3 tab of the downloaded eCQM Value Sets spreadsheet.
Review medications with all patients at every visit.
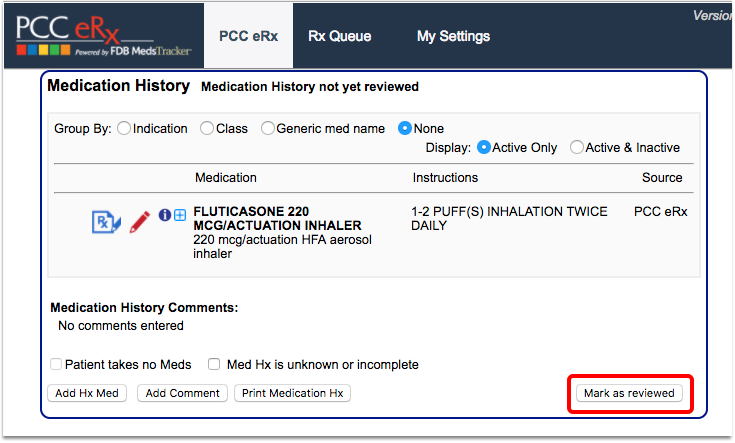
If a patient is prescribed asthma-related medications by a specialist or other clinician outside of your practice, update their medication history with that information.
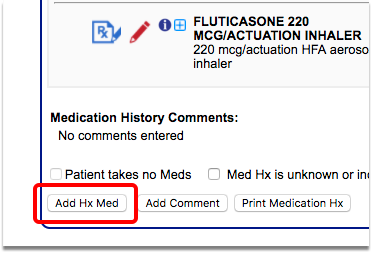
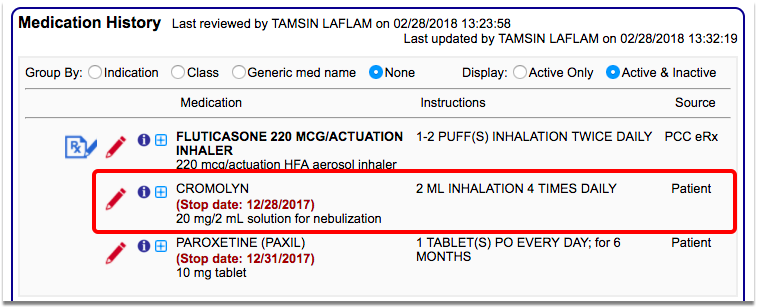
When you are finished charting each visit, remember to click “Bill” and select an appropriate visit encounter code. In addition to billing, the visit encounter code is used to calculate the CQM.
CMS136: ADHD: Follow-up Care for Children Prescribed Attention Deficit/Hyperactivity Disorder (ADHD) Medication
This measure calculates the percentage of children 6-12 years of age and newly dispensed a medication for attention-deficit/hyperactivity disorder (ADHD) who had appropriate follow-up care. Two rates are reported:
Measure 1 (Initiation Phase): Percentage of children who had one follow-up visit with a practitioner with prescribing authority during the 30-Day Initiation Phase.
Measure 2 (Continuation Phase): Percentage of children who remained on ADHD medication for at least 210 days and who, in addition to the visit in the Initiation Phase, had at least two additional follow-up visits with a practitioner within 270 days (9 months) after the Initiation Phase ended. (CMS at eCQI)
-
Denominator 1 (Initiation Phase): PCC EHR calculates the denominator of this measure by counting all patients who had an eligible encounter code billed on the electronic encounter form during the reporting period, who were between 6 and 12 years old, who were dispensed an ADHD medication 90 days before the start of the reporting period through 60 days after the start of the reporting period.
-
Denominator 2 (Continuation Phase): PCC EHR calculates the denominator of this measure by counting those patients from the Measure 1 denominator who remained on the ADHD medication for at least 210 days of the 300 days following the medication date.
-
Numerator 1 (Initiation Phase): PCC EHR calculates the numerator of this measure by counting all of the patients in the denominator who had at least one face-to-face visit with any EP within 30 days after the ADHD medication date.
-
Numerator 2 (Continuation Phase): PCC EHR calculates the numerator of this measure by counting all of the patients in the denominator who, in addition to the first visit during the Initiation Phase, had at least two additional follow-up visits with a clinician within 270 days (9 months).
-
Exclusions and Exceptions: Patients will be excluded from the denominator if they were actively on on an ADHD medication within the 120 days prior to the newly dispensed ADHD prescription; if they have a diagnosis of narcolepsy during or prior to the measurement period; and/or if they had an acute inpatient stay with a principal diagnosis of mental health or substance abuse during the 30 days after the ADHD medication date (for the Initiation Phase) or 300 days after the ADHD medication date (for the Continuation Phase).
Recommended PCC EHR Configuration for CMS136 ADHD Follow-up Care
There are no required PCC EHR configuration changes for recording data that will affect the ADHD Follow-up Care CQM.
Optionally, your practice may want to use a chart note protocol specifically for patients on ADHD medication that includes follow-up orders as a reminder to schedule visits into the future, depending on how long the patient is expected to be on the medication.
These options might help you to keep track of the patients that need follow-up visit, but will not affect this clinical quality measure.
Recommended Charting and Workflow for CMS136 ADHD Follow-up Care
When appropriate, use the PCC eRx section of the chart to prescribe ADHD-related medications.

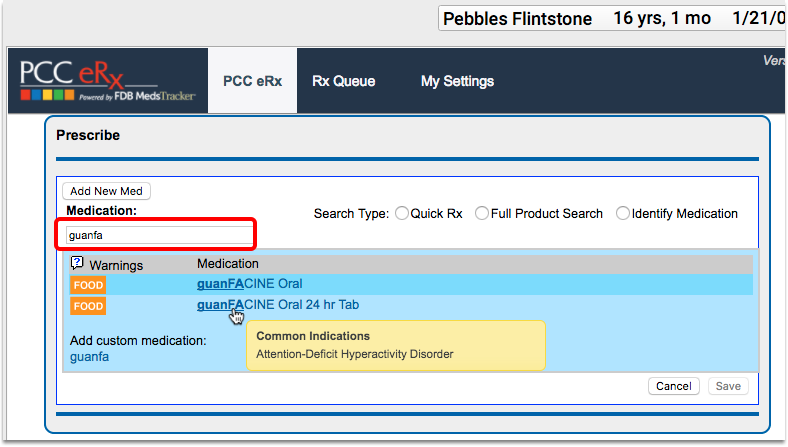
Which ADHD Medications Count for This CQM?: A number of medications count toward this measure, including dexmethylphenidate hydrochloride, methylphenidate, clonidine, and guanfacine. The NIH includes the full list of medications in its ADHD Medications value set, located on the VSAC website. You can also find the “ADHD Medications” value set within the CMS136v4 tab of the downloaded eCQM Value Sets spreadsheet.
Review medications with ADHD patients at every visit. If a patient is prescribed ADHD-related medications by a specialist or other clinician outside of your practice, update their medication history with that information.

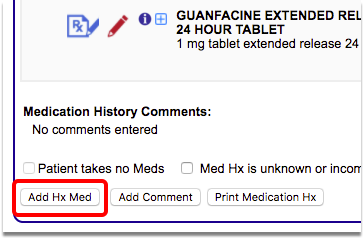
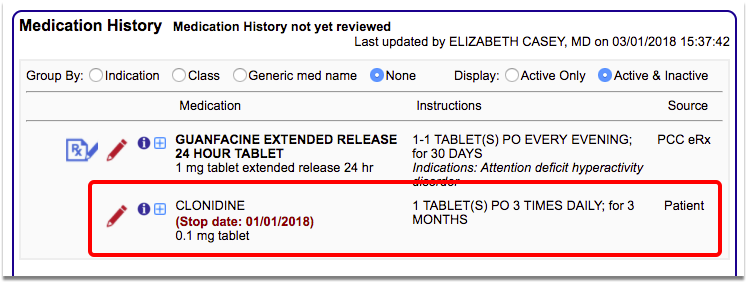
For patients on a newly prescribed ADHD medication, schedule at least one follow-up visit with a prescribing clinician during the 30-day Initiation Phase, dated from when the ADHD medication is dispensed.
You can use the Followup orders component to create a task for your nurse or scheduler to schedule another visit within 30 days.
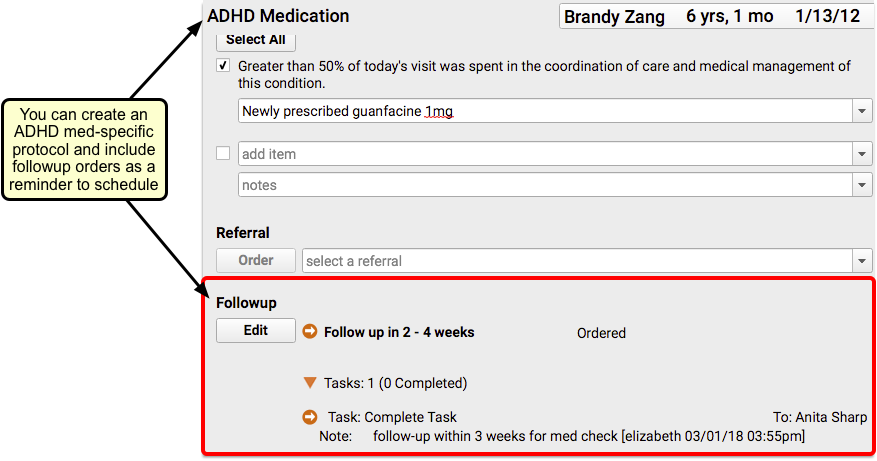
If the patient is remaining on ADHD medication for a longer period, schedule periodic follow-up visits with a prescribing clinician. Specifically, after the 30-day Initiation Phase, make certain the patient is seen for a follow-up at least twice within the following 9 months.
Follow-up visits during the Continuation Phase do not need to be with the same provider.
You can also use the Measure 1 (Initiation Phase) Details report as a recall tool to identify kids with newly prescribed ADHD meds during the reporting period, who will need follow-up visits scheduled.
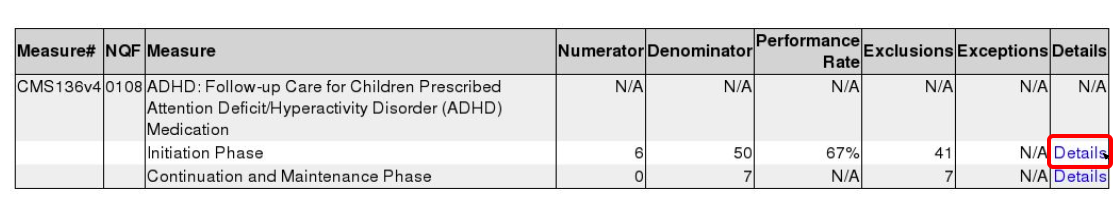
When you are finished charting each visit, remember to click “Bill” and select an appropriate visit encounter code. In addition to billing, the visit encounter code is used to calculate the CQM.
CMS146: Appropriate Testing for Children with Pharyngitis
This measure calculates the percentage of patients 2-18 years of age who were diagnosed with pharyngitis during the reporting period, were prescribed an antibiotic within 3 days, and received a group A streptococcus (strep) test. (CMS at eCQI)
-
Denominator: PCC EHR calculates the denominator of this measure by counting the number of visits for patients who had an eligible encounter code billed on the electronic encounter form OR an emergency department (ED) visit during the reporting period, who were between 2 and 18 years old, had a diagnosis of pharyngitis AND an antibiotic ordered on or three days after the visit.
-
Numerator: PCC EHR calculates the numerator of this measure by counting the number of visits for patients in the denominator who received a group A streptococcus (strep) test in the 7-day period of 3 days prior through 3 days after the diagnosis of pharyngitis.
-
Exclusions and Exceptions: Patients will be excluded from the denominator if they were taking antibiotics in the 30 days prior to the diagnosis of pharyngitis. Patients who were in hospice care during the measurement year are also excluded.
Recommended PCC EHR Configuration for CMS146 Appropriate Testing for Children with Pharyngitis
There are no required PCC EHR configuration changes for recording data that will affect the Appropriate Testing for Children with Pharyngitis CQM.
You may want to review your order configuration for group A streptococcus (Rapid Strep) orders, and/or edit your chart note protocols to make it easier to diagnose pharyngitis and create orders.

Which Codes Can I Use for Strep Test Orders?: Your LOINC lab test result codes must be taken from the Group A Streptococcus Test value set, from the NIH’s Value Set Authority Center. PCC recommends using “Streptococcus pyogenes Ag [Presence] in Unspecified specimen by Immunofluorescence”. You can also find the “Group A Streptococcus Test” value set within the CMS146v3 tab of the downloaded eCQM Value Sets spreadsheet.
Recommended Charting and Workflow for CMS146 Appropriate Testing for Children with Pharyngitis
When a patient visits your practice, chart any appropriate pharyngitis diagnoses in the Diagnoses component and/or the patient’s Problem List.
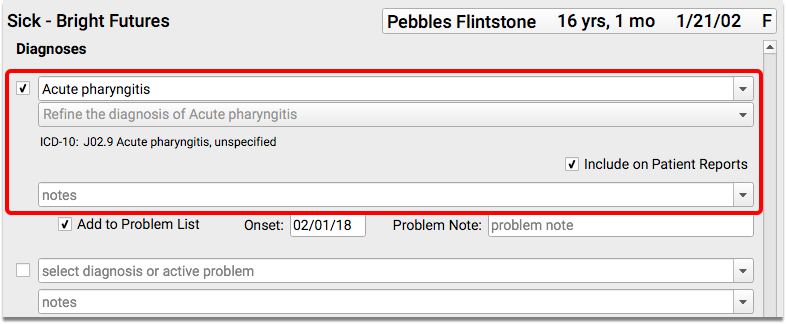
What Specific Diagnoses Count as Pharyngitis for this CQM?: You can select diagnoses from either the Acute Pharyngitis or the Acute Tonsillitis value sets, from the NIH’s Value Set Authority Center. Examples include: Acute pharyngitis, Acute tonsillitis, Streptococcal sore throat, and Viral pharyngitis. You can also find both the “Acute Pharyngitis” and the “Acute Tonsillitis” value sets within the CMS146v3 tab of the downloaded eCQM Value Sets spreadsheet.
When appropriate, create and complete lab orders to test for group A streptococcus and enter results in the lab order.
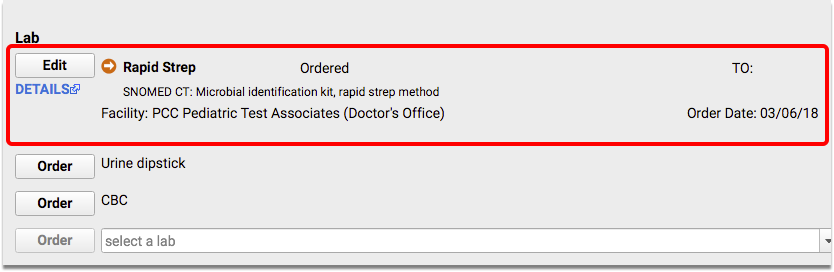
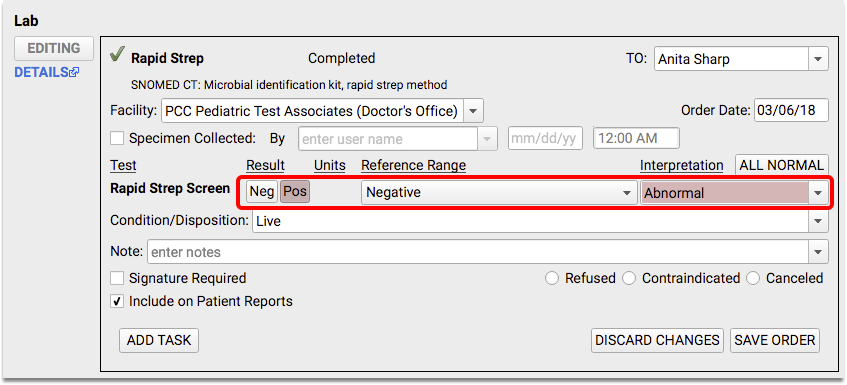
When appropriate, prescribe antibiotics. (To be included in the measure, antibiotic needs to be ordered on or within three days of the visit.)

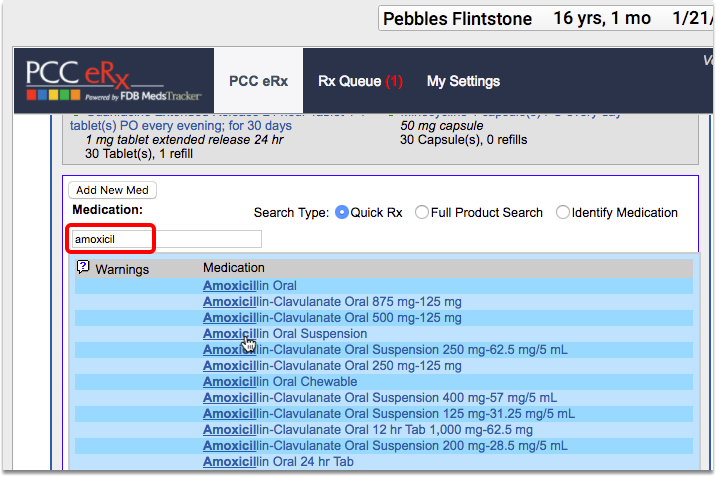
Which Antibiotics Count for This CQM?: A number of medications count toward this measure, including common antibiotics such as minocycline, azithromycin, doxycycline, and amoxicillin. The NIH includes the full list of antibiotics in its Antibiotic Medications for Pharyngitis value set, found on the VSAC website. You can also find the “Antibiotic Medications for Pharyngitis” value set within the CMS146v3 tab of the downloaded eCQM Value Sets spreadsheet.
Review medications at every visit. If a patient is prescribed antibiotics by a specialist or other clinician outside of your practice, update their medication history with that information.


When you are finished charting each visit, remember to click “Bill” and select an appropriate visit encounter code. In addition to billing, the visit encounter code is used to calculate the CQM.
CMS153: Chlamydia Screening for Women
This measure calculates the percentage of women 16-24 years of age who were identified as sexually active and who had at least one visit with the clinician and at least one test for chlamydia during the measurement period. (CMS at eCQI)
-
Denominator: PCC EHR calculates the denominator of this measure by counting all female patients who had an eligible encounter code billed in the electronic encounter form during the reporting period, who were between 16 and 24 years old, and who were considered sexually active by evidence of a charted diagnosis, problem on the Problem List, billed diagnosis, lab test, order, or prescribed medication.
-
Numerator: PCC EHR calculates the numerator of this measure by counting all of the patients in the denominator who had a LOINC test for Chlamydia, generally inside a Chlamydia test lab order, with a positive or negative result, on an encounter date within the reporting period.
-
Exclusions: If a patient would be considered sexually active because of a pregnancy test, but they had a radiology LOINC test afterwards or were prescribed certain qualifying medications, they will be excluded from the denominator as the pregnancy test could have been done solely as a precautionary measure.
-
Exceptions: None.
Recommended PCC EHR Configuration for CMS153 Chlamydia Screening for Women
In order to properly record Chlamydia tests, your practice should review your lab order configuration and add appropriate LOINC tests to your order or orders.
Additionally, you might want to review the following optional steps:
- In order to chart sexual activity, your practice may want to make adjustments to your chart note protocols and add LOINC tests to pregnancy tests or other orders.
- Optionally, you may also wish to review and update Radiology orders to make sure they include appropriate LOINC tests so they can be counted by the report. Female patients with a pregnancy test followed by an x-ray are not considered sexually active for the purposes of this measure.
- Optionally, you can also update your practice’s chart note protocols to make it easier to record sexual activity (by adding default diagnoses to age-appropriate chart notes, for example) and order and administer a Chlamydia test (by adding it as a default test to age-appropriate chart notes).
Review and Update Chlamydia Lab Orders to Include LOINC Tests
Open the Lab Configuration Tool
Click on the Tools menu and select Lab Configuration.
Edit or Add Chlamydia Test Lab Order
Double-click on your Chlamydia test order, or click “Add” to create one.
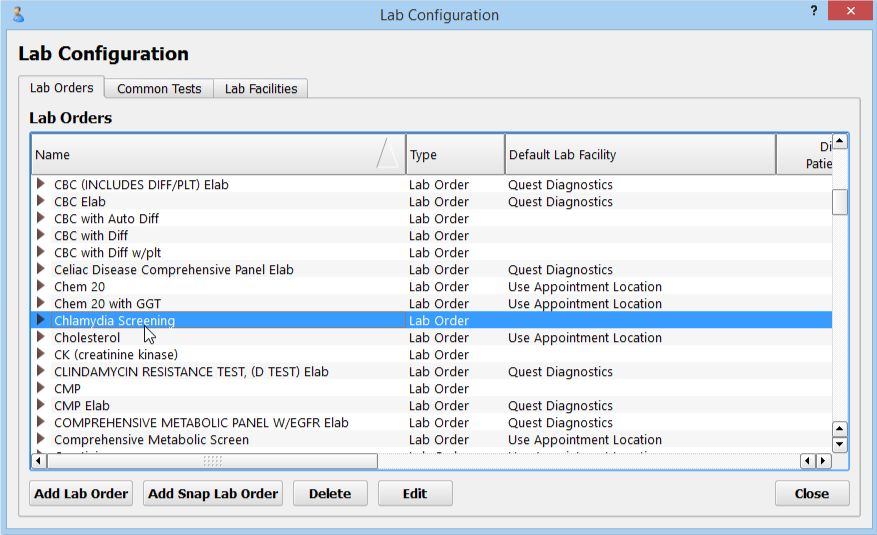
Configure Basic Order Details for Your Chlamydia Test Order
Review the order name and set any other configurable options. For example, you may want an order to be private by default, in which case you would deselect the “Include on Patient Reports” option.
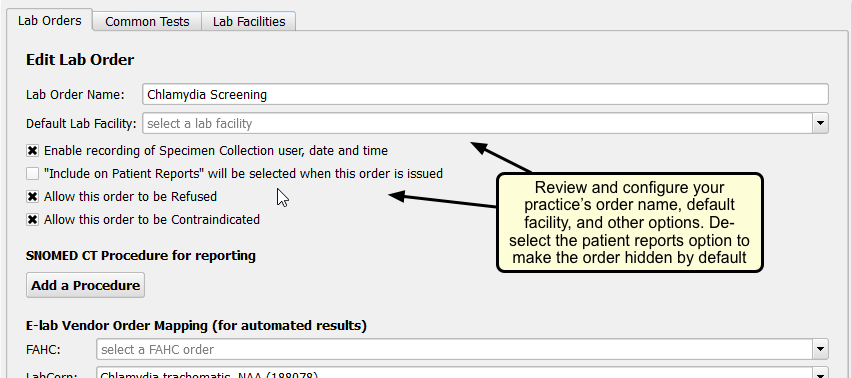
Review and/or Add Tests
Review tests for the order. To add a test, use the drop-down menu for each e-lab vendor or the manual result entry section.
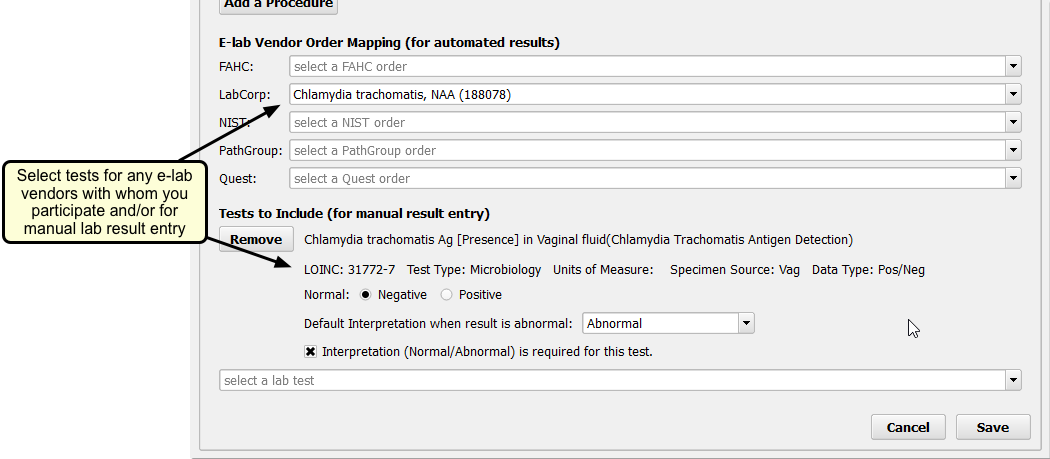
Which Codes Can I Use for Chlamydia Tests?: Your LOINC lab test result codes must be taken from the Chlamydia Screening value set, from the NIH’s Value Set Authority Center. One example is “Chlamydia trachomatis Ag Presence in Vaginal fluid”. You can also find the “Chlamydia Screening” value set within the CMS153v3 tab of the downloaded eCQM Value Sets spreadsheet.
Repeat for Other Lab Orders
If you have other chlamydia screening orders, such as an entry for e-labs and one for manually entered lab results, review each one and check that appropriate LOINC tests are tracked for each.
Recommended Charting and Workflow for CMS153 Chlamydia Screening for Women
When you see patients, chart any appropriate diagnoses that may indicate sexual activity, such as pregnancy, genital herpes, etc., in the Diagnoses component and/or the patient’s Problem List.
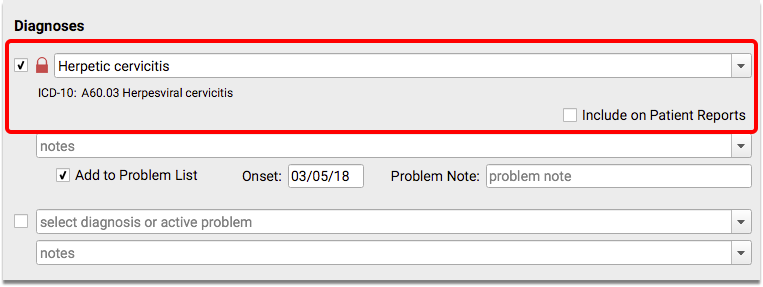
What Specific Diagnoses Indicate Sexual Activity for this CQM?: The Chlamydia value set includes a number of diagnoses that count for this measure. Diagnoses are also taken from the Complications of Pregnancy, Childbirth and the Puerperium, Genital Herpes, Gonococcal Infections and Venereal Diseases, HIV, Inflammatory Diseases of Female Reproductive Organs, Other Female Reproductive Conditions, and Syphilis value sets, all found on the VSAC website. All of these value sets are available within the CMS153v3 tab of the downloaded eCQM Value Sets spreadsheet.
You might also complete lab tests that indicate sexual activity, such as pregnancy tests.
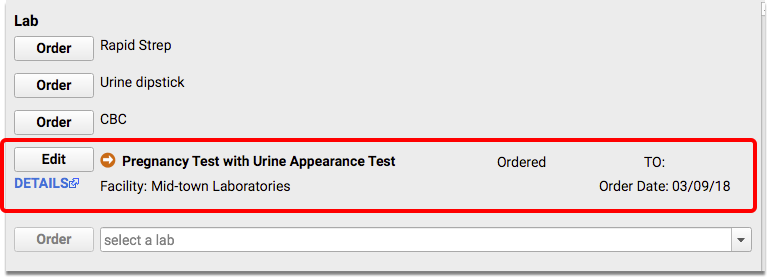
Which Lab Tests Might Indicate Sexual Activity for this CQM?: The Pregnancy Test value set includes lab tests that count for this measure. Lab tests are also taken from the Lab Tests During Pregnancy, Lab Tests for Sexually Transmitted Infections, and Pap Test value sets, all found on the VSAC website. All of these value sets are available within the CMS153v3 tab of the downloaded eCQM Value Sets spreadsheet.
In addition, some prescriptions that you order might indicate sexual activity, such as birth control pills.
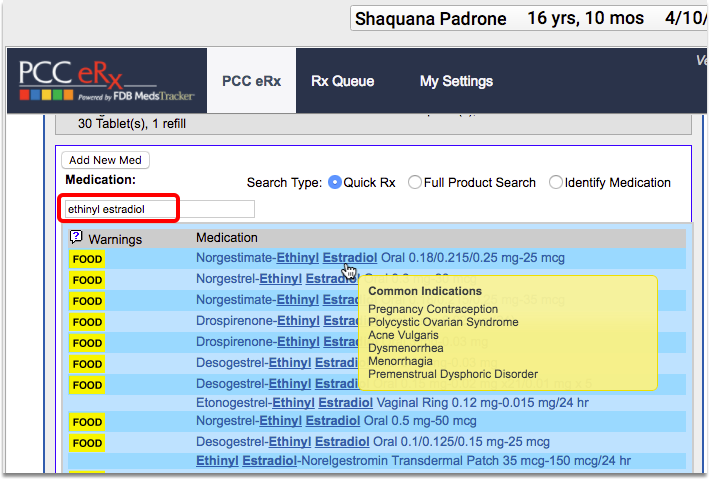
Which Medications Might Indicate Sexual Activity for this CQM?: The Contraceptive Medications value set includes medications that count for this measure. The Isotretinoin value set also includes prescriptions that count. Both of these value sets are found on the VSAC website. The “Contraceptive Medications” and “Isotretinoin” value sets are also available within the CMS153v3 tab of the downloaded eCQM Value Sets spreadsheet.
When appropriate, order a Chlamydia screening test in the Lab Orders component on the chart note. Later, enter results.
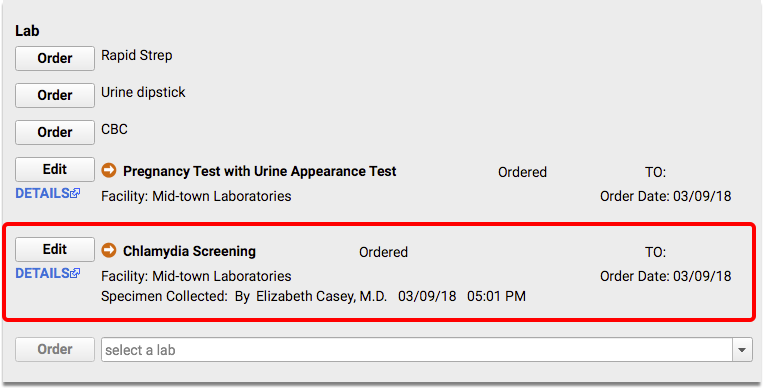
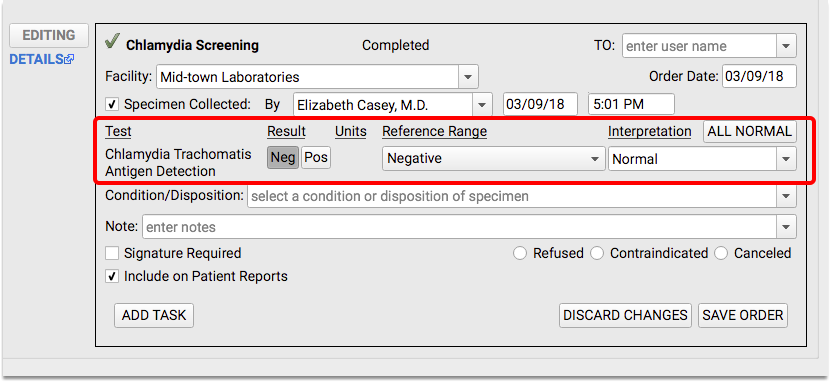
For each visit, make sure the correct Provider of Encounter clinician is indicated on the chart note.
When you are finished charting each visit, remember to click “Bill” and select an appropriate visit encounter code. In addition to billing, the visit encounter code is used to calculate the CQM.
CMS154: Appropriate Treatment for Children with Upper Respiratory Infection (URI)
This measure calculates the percentage of patients 3 months-18 years of age who were diagnosed with upper respiratory infection (URI) during the reporting period, and were not dispensed an antibiotic prescription within 3 days of the visit. (CMS at eCQI)
-
Denominator: PCC EHR calculates the denominator of this measure by counting the number of visits for patients who had an eligible encounter code billed on the electronic encounter form during the reporting period, who were between 3 months and 18 years old, and had a diagnosis of upper respiratory infection (URI).
-
Numerator: PCC EHR calculates the numerator of this measure by counting the number of visits for patients in the denominator who did not receive a prescription for antibiotic medication on or 3 days after the visit.
-
Exclusions and Exceptions: Patients will be excluded from the denominator if they were taking antibiotics in the 30 days prior to the diagnosis of URI.
Recommended PCC EHR Configuration for CMS154 Appropriate Treatment for Children with URI
There are no required PCC EHR configuration changes for recording data that will affect the Appropriate Testing for Children with Pharyngitis CQM.
You may want to edit your chart note protocols to make it easier to diagnose URI.
Recommended Charting and Workflow for CMS154 Appropriate Treatment for Children with URI
When you see patients, chart any appropriate URI diagnoses in the Diagnoses component and/or the patient’s Problem List.
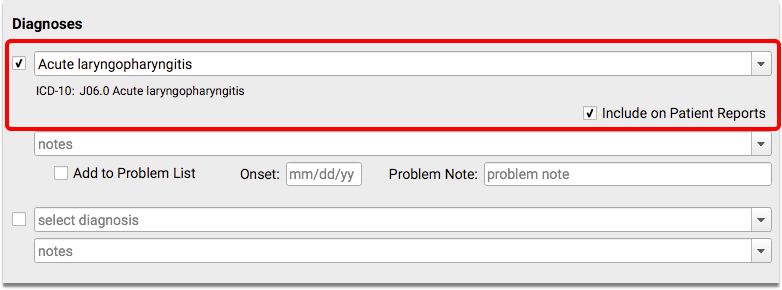
What Specific Diagnoses Count as URI for this CQM?: You can select diagnoses from the Upper Respiratory Infection value set, from the NIH’s Value Set Authority Center. Examples include: Acute upper respiratory infection and and Acute laryngopharyngitis. You can also find both the “Upper Respiratory Infection” value set within the CMS154v3 tab of the downloaded eCQM Value Sets spreadsheet.
When appropriate, prescribe antibiotics. (To be included in the measure, antibiotic needs to be ordered on or within three days of the visit.)


Which Antibiotics Count for This CQM?: A number of medications count toward this measure, including common antibiotics such as minocycline, azithromycin, doxycycline, and amoxicillin. The NIH includes the full list of antibiotics in its Antibiotic Medications for Pharyngitis value set, found on the VSAC website. You can also find the “Antibiotic Medications for Pharyngitis” value set within the CMS154v3 tab of the downloaded eCQM Value Sets spreadsheet.
Review medications at every visit. If a patient is prescribed antibiotics by a specialist or other clinician outside of your practice, update their medication history with that information.


When you are finished charting each visit, remember to click “Bill” and select an appropriate visit encounter code. In addition to billing, the visit encounter code is used to calculate the CQM.
CMS155: Weight Assessment and Counseling for Nutrition and Physical Activity for Children and Adolescents
This measure calculates the percentage of patients 3-17 years of age who had had a visit during the reporting period, and had their height, weight, and body mass index (BMI) documented, and/or received counseling for nutrition, and/or received counseling for physical activity. (CMS at eCQI)
-
Denominator: PCC EHR calculates the denominator of this measure by counting all patients who had an eligible encounter code billed on the electronic encounter form during the reporting period and who were between 3 and 17 years old.
-
Numerator 1: PCC EHR calculates the first numerator of this measure by counting all of the patients in the denominator who had a height, weight, and BMI percentile recorded during the measurement period.
-
Numerator 2: PCC EHR calculates the second numerator of this measure by counting all of the patients in the denominator who received counseling for nutrition during a visit that occurred within the measurement period.
-
Numerator 3: PCC EHR calculates the third numerator of this measure by counting all of the patients in the denominator who received counseling for physical activity during a visit that occurred within the measurement period.
-
Exclusions and Exceptions: Patients will be excluded from the denominator if they have an active diagnosis of pregnancy during the measurement period.
Recommended PCC EHR Configuration for CMS 155 Weight Assessment and Counseling
In order to chart counseling for nutrition or physical exercise, your practice can create medical procedure orders and add the specified SNOMED-CT procedures to those orders. Then you can add the orders to chart notes so they are easy to select at every visit.
For a step-by-step procedure on how to add codes to orders and add specific orders to chart notes, read Use Orders to Track Measures for Mandates.
Configure Your Nutrition Counseling Order
Create or edit a medical procedure order for nutrition counseling.
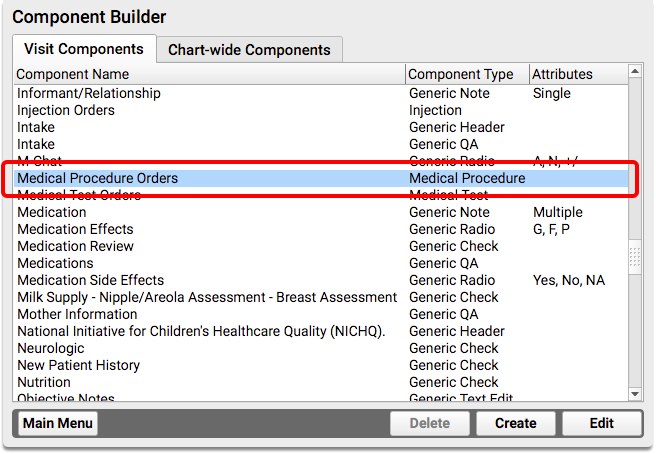
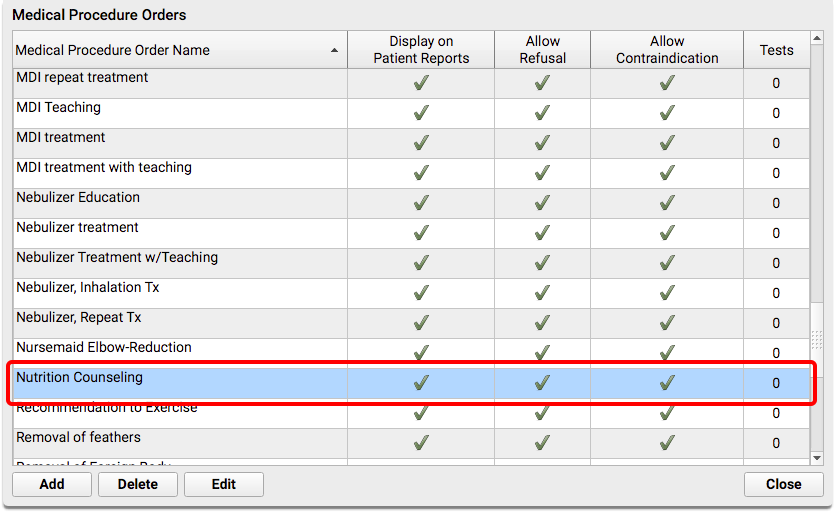
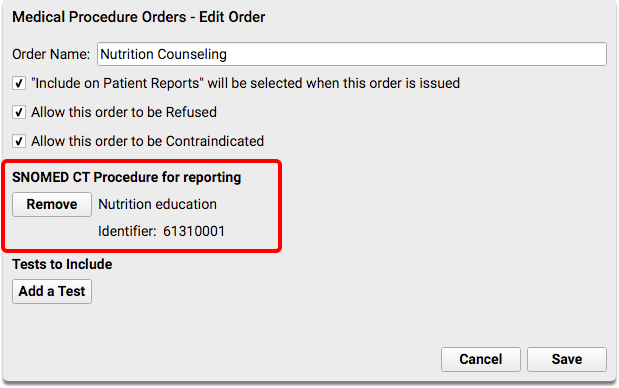
For the nutrition counseling order, you should select SNOMED-CT code 61310001, “Nutrition education”.
Configure Your Physical Activity Counseling Order
Create or edit a medical procedure order for physical activity counseling.

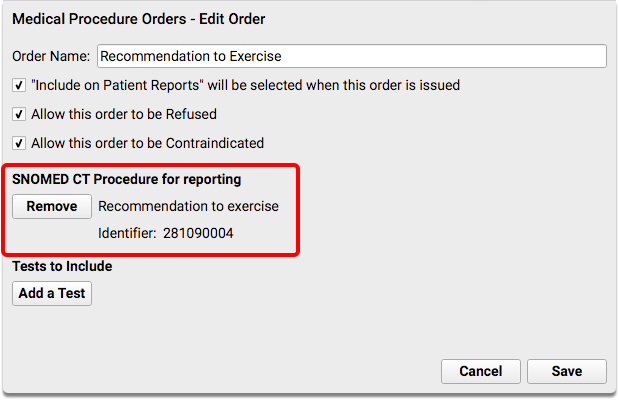
For the physical activity counseling order, you should select SNOMED-CT code 281090004, “Recommendation to exercise”.
Use the Specified SNOMED Codes: Please note that the 2018 ICD-10 code Z71.82, “Exercise counseling” will not work with PCC EHR reporting.
Add Nutrition and Physical Activity Counseling Orders to Your Chart Note Protocols
After you create the new medical procedure orders, you can add them to chart note protocols to make them easier to order. Your clinicians will then see the “Nutrition Counseling” order, for example, on every chart note.
For detailed instructions on how to add orders to a chart note protocol, read Use Orders to Track Measures for Mandates.
For each protocol, find or add the Medical Procedures Orders component, and then add the nutrition and physical exercise orders.
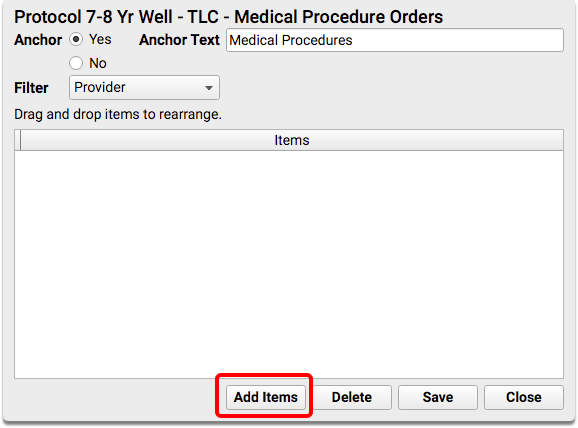
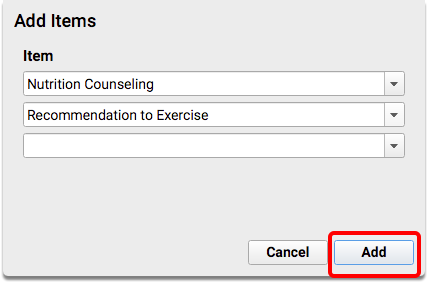
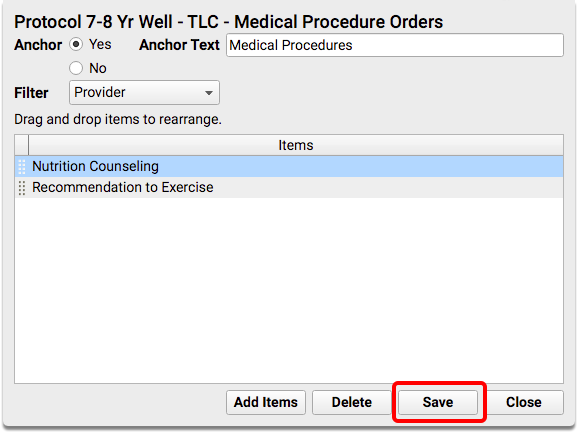
Recommended Charting and Workflow for CMS 155 Weight Assessment and Counseling
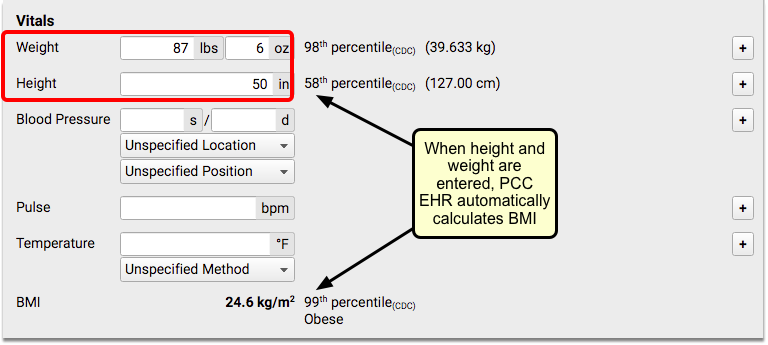
Collect height and weight during normal office visits, well exams and other appropriate visit types.
When appropriate, order your practice’s nutrition and/or physical activity counseling medical procedure.
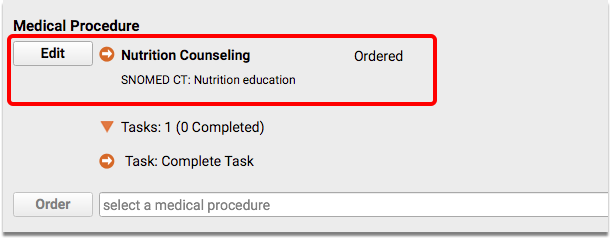
When you are finished charting, remember to click “Bill” and select an appropriate visit encounter code. In addition to billing, the visit encounter code is used to calculate the CQM.
PCC’s Current Certification Status and Required CQMs for PCMH
PCC EHR is Prevalidated for PCMH: By using PCC EHR, your practice is pre-validated for automatic credits towards PCMH recognition. Many pediatric practices have used PCC to achieve PCMH recognition.
Please contact PCC for help understanding and applying for PCMH programs in your state. PCC Support and our Pediatric Solutions team can show you what you need to apply and help you evaluate your options.
What CQMs Are You Required to Report On
You have several options for reporting on Clinical Quality Measures at your practice, depending on whether you applied for the EHR Medicaid Incentive Program or are applying for PCMH recognition.
Learn About PCMH Programs: Just getting started? Read Become a Patient Centered Medical Home (PCMH).
CQMs that Were Required for the EHR Medicaid Incentive Program
When you completed your Meaningful Use attestation each year, you calculated and submitted each clinician’s numbers for 9 Clinical Quality Measures, from a total of 64. Those nine measures needed to be drawn from at least three of six domains (Patient and Family Engagement, Population/Public Health, Patient Safety, Care Coordination, Efficient Use of Healthcare Resources, Clinical Process/Effectiveness).
In order to simplify the selection of measures, CMS identified a set of 9 CQMs for pediatric populations that meet all the requirements of the program. These recommended measures “focus on conditions that contribute to the morbidity and mortality of most Medicaid beneficiaries. They also focus on areas that represent national public health priorities or disproportionately drive health care costs.” (CMS.gov)
PCC built charting and workflow technologies, and our CQM report, around these 9 recommended pediatric CQMs.
Below are the 9 measures for which PCC EHR tracks and provides calculations under the EHR Medicaid Incentive Program 2014-edition CQM rules:
-
CMS2: Preventative Care and Screening: Screening for Clinical Depression and Follow-Up Plan
-
CMS75: Children Who Have Dental Decay or Cavities
-
CMS117: Childhood Immunization Status
-
CMS126: Use of Appropriate Medications for Asthma
-
CMS136: ADHD: Follow-Up Care for Children Prescribed Attention-Deficit/Hyperactivity Disorder (ADHD) Medication
-
CMS146: Appropriate Testing for Children with Pharyngitis
-
CMS153: Chlamydia Screening for Women
-
CMS155: Weight Assessment and Counseling for Nutrition and Physical Activity for Children and Adolescents
-
CMS154: Appropriate Treatment for Children with Upper Respiratory Infection (URI)
While you consider workflow and configuration adjustments, remember that there is no threshold for these measures; the program required that clinicians simply submit data as it pertains to each CQM.
CQMs for PCMH
There are many different ways a pediatric practice can achieve PCMH recognition. Reporting on CQM measures is not required. That being said, reporting on Clinical Quality Measures can help you complete element 6a of your PCMH application. It would be very difficult to proceed beyond PCMH recognition level 1 or level 2 without CQM reporting.
Element 6a requires that a practice measures and receives data on at least two immunization measures, at least two other preventive care measures, and at least three chronic or acute care clinical measures. Additionally, the performance data must be stratified for vulnerable populations.
The nine Pediatric CQMs described in the “CQMs For Meaningful Use” section above, and available in PCC EHR’s Clinical Quality Measures report, meet or exceed these requirements. However, your practice could choose other measures.
For example, you could use PCC’s Practice Vitals Dashboard to report on:
- Seasonal flu vaccine rates (vaccine measure)
- Asthma patients up-to-date on flu vaccine (vaccine measure)
- ADHD Followup Rate (chronic/acute measure)
- Well Visit Rates (preventive measure)
- Developmental screening rates (preventive measure)
For your PCMH application, your practice could use the 9 CMS recommended CQMs that are described in this document, or use data from Practice Vitals Dashboard to report on other CQMs, or use an entirely different set of CQMs, or forego CQM reporting altogether and aim for a lower level of PCMH recognition.
